Abstract
Background
The efficacy of different types of preoperative biliary drainage for cholangiocarcinoma has been debated over the past two decades. Controversy concerning the use of percutaneous transhepatic biliary drainage (PTBD) versus endoscopic biliary drainage (EBD) still exists. This study aimed to compare the long-term outcomes between PTBD and EBD in patients with distal cholangiocarcinoma.
Methods
Data of patients diagnosed with distal cholangiocarcinoma who underwent preoperative PTBD or EBD from January 1999 to December 2017 were analyzed retrospectively. Post-surgical outcomes, including the incidence of post-operative complications, peritoneal metastasis, disease-free survival, and overall survival, were analyzed. Survival analyses were also performed after propensity score matching in the PTBD and EBD groups.
Results
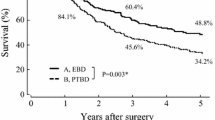
The incidence of post-operative complications was similar in both groups. The 5-year estimated cumulative incidences for peritoneal metastasis were 14.7% and 7.2% in the PTBD and EBD groups, respectively (p = 0.192). The 5-year disease-free survival rates were 23.7% and 47.3% in the PTBD and EBD groups, respectively (p = 0.015). In the multi-variate analysis for overall survival, PTBD was an independent poor prognostic factor. The 5-year overall survival rates were 35.9% and 56.3% in the PTBD and EBD groups, respectively (hazard ratio 1.85, confidence interval 1.05–3.26, p = 0.035). The results after propensity score matching indicated a poorer prognosis in the PTBD group, with a 5-year survival rate of 35.9% in the PTBD group vs 56.0% in the EBD group (p = 0.044).
Conclusion
PTBD should be considered as a negative prognostic factor in distal cholangiocarcinoma patients.





Similar content being viewed by others
Change history
20 July 2021
A Correction to this paper has been published: https://doi.org/10.1007/s10147-021-01975-z
References
Fang Y, Gurusamy KS, Wang Q et al (2013) Meta-analysis of randomized clinical trials on safety and efficacy of biliary drainage before surgery for obstructive jaundice. Br J Surg 100(12):1589–1596
van der Gaag NA, Rauws EA, van Eijck CH et al (2010) Preoperative biliary drainage for cancer of the head of the pancreas. N Engl J Med 362:129–137
Sewnath ME, Karsten TM, Prins MH et al (2002) A meta-analysis on the efficacy of preoperative biliary drainage for tumors causing obstructive jaundice. Ann Surg 236(1):17–27
Miyazaki M, Yoshitomo H, Miyakawa S et al (2015) Clinical practice guidelines for the management of biliary tract cancers 2015: the 2nd English edition. J Hepatobiliary Pancreat Sci 22:249–273
Kawai M, Kondo S, Yamaue H et al (2011) Predictive risk factors for clinically relevant pancreatic fistula analyzed in 1,239 patients with pancreaticoduodenectomy: multicenter data collection as a project study of pancreatic surgery by the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci 18(4):601–608
Choi YM, Cho EH, Lee KY et al (2008) Effect of preoperative biliary drainage on surgical results after pancreaticoduodenectomy in patients with distal common bile duct cancer: focused on the rate of decrease in serum bilirubin. World J Gastroenterol 14(7):1102–1107
Hirano S, Tanaka E, Tsuchikawa T et al (2014) Oncological benefit of preoperative endoscopic biliary drainage in patients with hilar cholangiocarcinoma. J Hepatobiliary Pancreat Sci 21(8):533–540
Komaya K, Ebata T, Yokoyama Y et al (2017) Verification of the oncologic inferiority of percutaneous biliary drainage to endoscopic drainage: a propensity score matching analysis of resectable perihilar cholangiocarcinoma. Surgery 161(2):394–404
Higuchi R, Yazawa T, Uemura S et al (2017) ENBD is associated with decreased tumor dissemination compared to PTBD in perihilar cholangiocarcinoma. J Gastrointest Surg 21(9):1506–1514
Wiggers JK, Groot Koerkamp B, Coelen RJ et al (2015) Percutaneous preoperative biliary drainage for resectable perihilar cholangiocarcinoma: no association with survival and no increase in seeding metastases. Ann Surg Oncol 22(Suppl 3):S1156–S1163
Komaya K, Ebata T, Fukami Y et al (2016) Percutaneous biliary drainage is oncologically inferior to endoscopic drainage: a propensity score matching analysis in resectable distal cholangiocarcinoma. J Gastroenterol 51(6):608–619
Mori S, Aoki T, Park KH et al (2019) Impact of preoperative percutaneous transhepatic biliary drainage on post-operative survival in patients with distal cholangiocarcinoma. ANZ J Surg 89(9):E363–E367
Lee H, Han Y, Kim JR et al (2018) Preoperative biliary drainage adversely affects surgical outcomes in periampullary cancer: a retrospective and propensity score-matched analysis. J Hepatobiliary Pancreat Sci 25(3):206–213
National Cancer Institute (2020) SEER cancer stat facts: pancreatic cancer. https://seer.cancer.gov/statfacts/html/pancreas.html. Accessed Dec 2020
Banales JM, Cardinale V, Carpino G et al (2016) Expert consensus document: cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European Network for the Study of Cholangiocarcinoma (ENS-CCA). Nat Rev Gastroenterol Hepatol 13(5):261–280
National Cancer Center (Ministry of Health, Labour and Welfare, National Cancer Registry) (2020) Cancer registry and statistics. Cancer information service. https://ganjoho.jp/data/reg_stat/statistics/dl/cancer_incidenceNCR(2016-2017).xls. Accessed Dec 2020
Razumilava N, Gores GJ (2014) Cholangiocarcinoma. Lancet 383(9935):2168–79
Mosadeghi S, Liu B, Bhuket T et al (2016) Sex-specific and race/ethnicity-specific disparities in cholangiocarcinoma incidence and prevalence in the USA: an updated analysis of the 2000–2011 surveillance, epidemiology and end results registry. Hepatol Res 246(7):669–677
Hashimoto S, Ito K, Koshida S et al (2016) Risk factors for post-endoscopic retrograde cholangiopancreatography (ERCP) pancreatitis and stent dysfunction after preoperative biliary drainage in patients with malignant biliary stricture. Intern Med 55(18):2529–2536
Sasahira N, Hamada T, Togawa O et al (2016) Multicenter study of endoscopic preoperative biliary drainage for malignant distal biliary obstruction. World J Gastroenterol 22(14):3793–3802
Bassi C, Marchegiani G, Dervenis C et al (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery 161(3):584–591
Amin MB, Gress DM (2017) AJCC cancer staging manual, 8th edn. Springer, New York
Japanese Society of Hepato-Biliary-Pancreatic Surgery (2013) General rules for surgical and pathological studies on cancer of the biliary tract, 6th edn. Kanehara, Tokyo (in Japanese)
Wakai T, Sakata J, Katada T et al (2018) Surgical management of carcinoma in situ at ductal resection margins in patients with extrahepatic cholangiocarcinoma. Ann Gastroenterol Surg 2(5):359–366
Park Y, Hwang DW, Kim JH et al (2019) Prognostic comparison of the longitudinal margin status in distal bile duct cancer: R0 on first bile duct resection versus R0 after additional resection. J Hepatobiliary Pancreat Sci 26(5):169–178
Rubin DB (1997) Estimating causal effects from large data sets using propensity scores. Ann Intern Med 127:757–763
Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivariate Behav Res 46(3):399–424
Tanaka N, Nobori M, Suzuki Y (1997) Does bile spillage during an operation present a risk for peritoneal metastasis in bile duct carcinoma? Surg Today 27(11):1010–1014
Blakely AM, Wong P, Chu P et al (2019) Intraoperative bile spillage is associated with worse survival in gallbladder adenocarcinoma. J Surg Oncol 120(4):603–610
Miura F, Sano K, Wada K et al (2017) Prognostic impact of type of preoperative biliary drainage in patients with distal cholangiocarcinoma. Am J Surg 214(2):256–261
Hu QL, Liu JB, Ellis RJ et al (2020) Association of preoperative biliary drainage technique with postoperative outcomes among patients with resectable hepatobiliary malignancy. HPB (Oxford) 22(2):249–257
Kawakami H, Kuwatani M, Onodera M et al (2011) Endoscopic nasobiliary drainage is the most suitable preoperative biliary drainage method in the management of patients with hilar cholangiocarcinoma. J Gastroenterol 46(2):242–248
Choi SH, Gwon DI, Ko GY et al (2011) Hepatic arterial injuries in 3110 patients following percutaneous transhepatic biliary drainage. Radiology 261(3):969–975
Kochar B, Akshintala VS, Afghani E et al (2015) Incidence, severity, and mortality of post-ERCP pancreatitis: a systematic review by using randomized, controlled trials. Gastrointest Endosc 81(1):143-149.e9
Andriulli A, Loperfido S, Napolitano G et al (2007) Incidence rates of post-ERCP complications: a systematic survey of prospective studies. Am J Gastroenterol 102(8):1781–1788
Asari S, Matsumoto I, Ajiki T et al (2015) Perioperative management for pancreatoduodenectomy following severe acute pancreatitis in patients with periampullary cancer: our experience with six consecutive cases. Surg Today 45(2):181–188
Murray B, Carter R, Imrie C et al (2003) Diclofenac reduces the incidence of acute pancreatitis after endoscopic retrograde cholangiopancreatography. Gastroenterology 124(7):1786–1791
Elmunzer BJ, Waljee AK, Elta GH et al (2008) A meta-analysis of rectal NSAIDs in the prevention of post-ERCP pancreatitis. Gut 57(9):1262–1267
Mazaki T, Masuda H, Takayama T (2010) Prophylactic pancreatic stent placement and post-ERCP pancreatitis: a systematic review and meta-analysis. Endoscopy 42:842–853
Kawakami H, Kondo S, Kuwatani M et al (2011) Preoperative biliary drainage for hilar cholangiocarcinoma: which stent should be selected? J Hepatobiliary Pancreat Sci 18(5):630–635
Coelen RJS, Roos E, Wiggers JK et al (2018) Endoscopic versus percutaneous biliary drainage in patients with resectable perihilar cholangiocarcinoma: a multicentre, randomised controlled trial. Lancet Gastroenterol Hepatol 3(10):681–690
Acknowledgements
The authors would like to express our gratitude to Kenichiro Imai, Hideki Kajiyama, Mimi Okano, Dr. Cao Manh-Thau, and Dr. Pipit Burasakarn for providing surgical assistance.
Funding
This work was supported by the JSPS KAKENHI under Grant number 18K08632 (non-restricted educational grand).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No author has any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10147_2021_1926_MOESM3_ESM.docx
Supplementary file3 (DOCX 16 KB) Supplementary Fig. 1 Kaplan-Meier curves for overall survival in patients without PBD or with PBD for distal cholangiocarcinoma
10147_2021_1926_MOESM4_ESM.docx
Supplementary file4 (DOCX 19 KB) Supplementary Fig. 2 Kaplan-Meier curves for disease-free survival after propensity score matching in patients who underwent percutaneous transhepatic biliary drainage or endoscopic biliary drainage for distal cholangiocarcinoma
About this article
Cite this article
Matsunaga, Y., Higuchi, R., Yazawa, T. et al. Negative prognostic outcomes of percutaneous transhepatic biliary drainage in distal cholangiocarcinoma: a retrospective analysis using propensity score matching. Int J Clin Oncol 26, 1492–1499 (2021). https://doi.org/10.1007/s10147-021-01926-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-021-01926-8