Abstract
Purpose of Review
Tuberculous meningitis (TBM) in children may mimic bacterial meningitis in the early stages. Being a subacute illness, early symptoms may be missed leading to clinical deterioration and late presentation. This review helps to highlight the clinical manifestations, newer diagnostic tests, and newer treatment guidelines of TBM in children.
Recent Findings
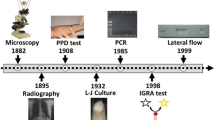
Newer tests like nuclei acid amplification tests (NAATs), line probe assays (LPAs), MGIT, antigen detection, and biomarkers are now available on cerebrospinal fluid (CSF) to aid diagnosis to help provide early management and prevent complications. Recent studies have helped optimize the treatment of TBM to prevent long-term neurological sequelae. Co-infection with HIV requires prompt treatment with anti-tubercular drugs and combination antiretroviral therapy.
Summary
With early diagnosis and prompt treatment, the risk of death can be reduced and neurological outcome improved.
Similar content being viewed by others
References
Global Tuberculosis Report 2019. Geneva. World Health Organization 2019. Available online from URL: https://apps.who.int/iris/bitstream/handle/10665/329368/9789241565714-eng.pdf?ua=1 [Accessed on 18th November 2019].
Chiang SS, Khan FA, Milstein MB, Tolman AW, Benedetti A, Starke JR, et al. Treatment outcomes of childhood tuberculous meningitis: a systematic review and meta-analysis. Lancet Infect Dis. 2014;14:947–57.
Rock RB, Olin M, Baker CA, Molitor TW, Peterson PK. Central nervous system tuberculosis: pathogenesis and clinical aspects. Clin Microbiol Rev. 2008;21(2):243–61.
Rich AR, McCordock HA. Pathogenesis of tubercular meningitis. Bull John Hopkins Hosp. 1933;52:5–13.
Isabel BE, Rogelio HP. Pathogenesis and immune response in tuberculous meningitis. Malays J Med Sci. 2014;21(1):4–10.
Be NA, Kim KS, Bishai WR, Jain SK. Pathogenesis of central nervous system tuberculosis. Curr Mol Med. 2009;9(2):94–9.
Torok ME. Tuberculous meningitis: advance in diagnosis and treatment. Br Med Bull. 2015;113:117–31.
Miftode EG, Domeanu OS, Leca DA, Juganariu G, Teodor A, Hurmuzache M, et al. Tuberculous meningitis in children and adults: a 10-year retrospective comparative analysis. PLoS One. 2015;10(7):e0133477.
Mezochow A, Thakur K, Vinnard C. Tuberculous meningitis in children and adults: new insights for an ancient foe. Curr Neurol Neurosci Rep. 2017;17(11):85.
Raut T, Garg RK, Jain A, Verma R, Singh MK, Malhotra HS, et al. Hydrocephalus in tuberculous meningitis: incidence, its predictive factors and impact on the prognosis. J Inf Secur. 2013;66(4):330–7.
Thwaites GE, Simmons CP, Than Ha Quyen N, Thi Hong Chau T, Phuong Mai P, Thi Dung N, et al. Pathophysiology and prognosis in Vietnamese adults with tuberculous meningitis. J Infect Dis. 2003;188:1105–15.
Simmons CP, Thwaites CP, Than Ha Quyen N, et al. The clinical benefit of adjunctive dexamethasone in tuberculous meningitis is not associated with measurable attenuation of peripheral or local immune responses. J Immunol. 2005;175:579–90.
Thwaites GE, Chau TT, Farrar JJ. Improving the bacteriological diagnosis of tuberculous meningitis. J Clin Microbiol. 2004;42:378–9.
Global laboratory initiative. Line probe assays for drug-resistant tuberculosis detection. Interpretation and reporting guide for laboratory staff and clinicians. Global TB Programme. World Health Organization. Geneva. Available online from : http://www.stoptb.org/wg/gli/assets/documents/LPA_test_web_ready.pdf [Accessed on 18th November 2019.]
Haldar S, Sankhyan N, Saharma N, Bansal A, Janin V, Gupta VK, et al. Detection of Mycobacterium tuberculosis GlcB or HspX antigens or devR DNA impacts the rapid diagnosis of tuberculous meningitis in children. PLoS One. 2012;7(9):e44630.
Kataria J, Rukmangadachar LA, Hariprasad G, O J, Tripathi M, Srinivasan A. Two dimensional difference gel electrophoresis analysis of cerebrospinal fluid in tuberculous meningitis patients. J Proteomics. 2011;74(10):2194–203.
Treatment of TB in Children. In World Health Organization. Guidance for national tuberculosis programmes on the management of tuberculosis in children. 2nd edition. 2014. Geneva. Available on URL: https://apps.who.int/iris/bitstream/handle/10665/112360/9789241548748_eng.pdf;jsessionid=053C9EA7991D9D49FFEC6BAA2F4C7361?sequence=1 [Accessed on 17th November 2019].
Ruslami R, Ganiem AR, Dian S, Apriani L, Achmad TH, van der Ven AJ, et al. Intensified regimen containing rifampicin and moxifloxacin for tuberculous meningitis: an open-label, randomised controlled phase 2 trial. Lancet Infect Dis. 2013;13(1):27–35.
Thwaites GE, Bhavnani SM, Chau TT, Hammel JP, Török ME, Van Wart SA, et al. Randomized pharmacokinetic and pharmacodynamic comparison of fluoroquinolones for tuberculous meningitis. Antimicrob Agents Chemother. 2011;55(7):3244–53.
Savic RM, Ruslami R, Hibma J, Hesseling A, Ramachandra G, Ganiem R, et al. Pediatric tuberculous meningitis: model-based approach to determining optimal doses of the anti- tuberculosis drugs rifampicin and levofloxacin for children. Clin Pharmacol Ther. 2015;98(6):622–9.
Prasad K, Singh MB, Ryan H. Corticosteroids for managing tuberculous meningitis. Cochrane Database Syst Rev. 2016;4:CD002244.
Shah I, Meshram L. High dose versus low dose steroids in children with tuberculous meningitis. J Clin Neurosci. 2014;21(5):761–4.
Schoeman JF, Springer P, Ravenscroft A, Donald P, Bekker LG, van Rensber AJ, et al. Adjunctive thalidomide therapy of childhood tuberculous meningitis: possible anti-inflammatory role. J Child Neurol. 2000;15:497–503.
Schoeman JF, Springer P, van Rensberg AJ, Swanevelder S, Hanekom WA, Haslett PAJ, et al. Adjunctive thalidomide therapy for childhood tuberculosis meningitis: results of a randomized study. J Child Neurol. 2004;19:250–7.
Panel on opportunistic infections in HIV-exposed and HIV-infected children. Guidelines for the prevention and treatment of opportunistic infections in HIV-exposed and HIV-infected children. 2013. Department of Health and Human Services. pV1–20. Available at https://aidsinfo.nih.gov/contentfiles/lvguidelines/oi_guidelines_pediatrics.pdf [Accessed on 18th November 2019].
Kalita J, Misra UK, Ranjan P. Predictors of long-term neurological sequelae of tuberculous meningitis: a multivariate analysis. Eur J Neurol. 2007 Jan;14(1):33–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Pediatric Infectious Diseases
Rights and permissions
About this article
Cite this article
Shah, I., Pereira, N.M.D. Tuberculous Meningitis in Children: a Review Article. Curr Infect Dis Rep 22, 11 (2020). https://doi.org/10.1007/s11908-020-0720-7
Published:
DOI: https://doi.org/10.1007/s11908-020-0720-7