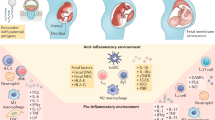
Abstract
The management of inflammatory rheumatic diseases during pregnancy and breastfeeding has undergone considerable change in the past few years. Modern therapeutics, including biologic and targeted synthetic DMARDs, have enabled substantial improvements in the control of rheumatic diseases, resulting in more patients with severe disease considering pregnancy. Therefore, management of disease for these patients needs to be discussed with clinicians before, during and after pregnancy and patients need to know what complications they might experience before they become pregnant. This Review summarizes the effects pregnancy has on various rheumatic diseases and the effects these diseases have on pregnancy, as well as providing advice regarding the alteration and monitoring of therapy before, during and after pregnancy.
Key points
-
Various inflammatory rheumatic diseases carry an increased burden of adverse pregnancy outcomes.
-
Pregnancy can exacerbate some but not all inflammatory rheumatic diseases.
-
Pre-pregnancy counselling is required to evaluate and reduce risks of adverse pregnancy outcomes for each patient.
-
Some therapies must be altered before, during and/or after pregnancy.
-
Careful monitoring is required throughout pregnancy by a multidisciplinary team.
-
Vigilance for disease flare is required post-partum.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Symmons, D. et al. The prevalence of rheumatoid arthritis in the United Kingdom: new estimates for a new century. Rheumatology 41, 793–800 (2002).
Rees, F. et al. The incidence and prevalence of systemic lupus erythematosus in the UK, 1999–2012. Ann. Rheum. Dis. 75, 136–141 (2016).
Ogdie, A. et al. Prevalence and treatment patterns of psoriatic arthritis in the UK. Rheumatology 52, 568–575 (2013).
Haroon, N. N., Paterson, J. M., Li, P. & Haroon, N. Increasing proportion of female patients with ankylosing spondylitis: a population-based study of trends in the incidence and prevalence of AS. BMJ Open 4, e006634 (2014).
Royle, J. G., Lanyon, P. C., Grainge, M. J., Abhishek, A. & Pearce, F. A. The incidence, prevalence, and survival of systemic sclerosis in the UK Clinical Practice Research Datalink. Clin. Rheumatol. 37, 2103–2111 (2018).
Ostensen, M. et al. State of the art: reproduction and pregnancy in rheumatic diseases. Autoimmun. Rev. 14, 376–386 (2015).
Flint, J. et al. BSR and BHPR guideline on prescribing drugs in pregnancy and breastfeeding— part I: standard and biologic disease modifying anti-rheumatic drugs and corticosteroids. Rheumatology 55, 1693–1697 (2016).
Flint, J. et al. BSR and BHPR guideline on prescribing drugs in pregnancy and breastfeeding— part II: analgesics and other drugs used in rheumatology practice. Rheumatology 55, 1698–1702 (2016).
Gotestam Skorpen, C. et al. The EULAR points to consider for use of antirheumatic drugs before pregnancy, and during pregnancy and lactation. Ann. Rheum. Dis. 75, 795–810 (2016).
de Man, Y. A. et al. Association of higher rheumatoid arthritis disease activity during pregnancy with lower birth weight: results of a national prospective study. Arthritis Rheum. 60, 3196–3206 (2009).
Clowse, M. E. B., Magder, L. S., Witter, F. & Petri, M. The impact of increased lupus activity on obstetric outcomes. Arthritis Rheum. 52, 514–521 (2005).
Ko, H. S. et al. Pregnancy outcomes and appropriate timing of pregnancy in 183 pregnancies in Korean patients with SLE. Int. J. Med. Sci. 8, 577–583 (2011).
Urowitz, M. B., Gladman, D. D., Farewell, V. T., Stewart, J. & Mcdonald, J. Lupus and pregnancy studies. Arthritis Rheum. 36, 1392–1397 (1993).
Chakravarty, E. F. et al. Factors that predict prematurity and preeclampsia in pregnancies that are complicated by systemic lupus erythematosus. Am. J. Obstet. Gynecol. 192, 1897–1904 (2005).
Cortes-Hernandez, J. et al. Clinical predictors of fetal and maternal outcome in systemic lupus erythematosus: a prospective study of 103 pregnancies. Rheumatology 41, 643–650 (2002).
Clowse, M. E. B., Magder, L., Witter, F. & Petri, M. Hydroxychloroquine in lupus pregnancy. Arthritis Rheum. 54, 3640–3647 (2006).
Andreoli, L. et al. EULAR recommendations for women’s health and the management of family planning, assisted reproduction, pregnancy and menopause in patients with systemic lupus erythematosus and/or antiphospholipid syndrome. Ann. Rheum. Dis. 76, 476–485 (2017).
Clowse, M. E., Chakravarty, E., Costenbader, K. H., Chambers, C. & Michaud, K. Effects of infertility, pregnancy loss, and patient concerns on family size of women with rheumatoid arthritis and systemic lupus erythematosus. Arthritis Care Res. 64, 668–674 (2012).
Helland, Y., Dagfinrud, H. & Kvien, T. K. Perceived influence of health status on sexual activity in RA patients: associations with demographic and disease-related variables. Scand. J. Rheumatol. 37, 194–199 (2008).
Schmidt, R. J. & Holley, J. L. Fertility and contraception in end-stage renal disease. Adv. Ren. Replace Ther. 5, 38–44 (1998).
Morel, N. et al. Study of anti-Mullerian hormone and its relation to the subsequent probability of pregnancy in 112 patients with systemic lupus erythematosus, exposed or not to cyclophosphamide. J. Clin. Endocrinol. Metab. 98, 3785–3792 (2013).
Khnaba, D. et al. Sexual dysfunction and its determinants in Moroccan women with rheumatoid arthritis. Pan Afr. Med. J. 24, 16 (2016).
Hansen, K. R. et al. A new model of reproductive aging: the decline in ovarian non-growing follicle number from birth to menopause. Hum. Reprod. 23, 699–708 (2008).
Ostensen, M. Sexual and reproductive health in rheumatic disease. Nat. Rev. Rheumatol. 13, 485–493 (2017).
Martinez, F. Update on fertility preservation from the Barcelona International Society for Fertility Preservation-ESHRE-ASRM 2015 expert meeting: indications, results and future perspectives. Hum. Reprod. 32, 1802–1811 (2017).
Chakravarty, E. F., Nelson, L. & Krishnan, E. Obstetric hospitalizations in the United States for women with systemic lupus erythematosus and rheumatoid arthritis. Arthritis Rheum. 54, 899–907 (2006).
Lin, H. C., Chen, S. F., Lin, H. C. & Chen, Y. H. Increased risk of adverse pregnancy outcomes in women with rheumatoid arthritis: a nationwide population-based study. Ann. Rheum. Dis. 69, 715–717 (2010).
Skomsvoll, J. F., Ostensen, M., Irgens, L. M. & Baste, V. Obstetrical and neonatal outcome in pregnant patients with rheumatic disease. Scand. J. Rheumatol. Suppl. 107, 109–112 (1998).
Wolfberg, A. J., Lee-Parritz, A., Peller, A. J. & Lieberman, E. S. Association of rheumatologic disease with preeclampsia. Obstet. Gynecol. 103, 1190–1193 (2004).
Reed, S. D., Vollan, T. A. & Svec, M. A. Pregnancy outcomes in women with rheumatoid arthritis in Washington State. Matern. Child Health J. 10, 361–366 (2006).
Zbinden, A., van den Brandt, S., Ostensen, M., Villiger, P. M. & Forger, F. Risk for adverse pregnancy outcome in axial spondyloarthritis and rheumatoid arthritis: disease activity matters. Rheumatology 57, 1235–1242 (2018).
Bowden, A. P., Barrett, J. H., Fallow, W. & Silman, A. J. Women with inflammatory polyarthritis have babies of lower birth weight. J. Rheumatol. 28, 355–359 (2001).
Clowse, M. E., Jamison, M., Myers, E. & James, A. H. A national study of the complications of lupus in pregnancy. Am. J. Obstet. Gynecol. 199, 5 (2008).
Buyon, J. P. et al. Predictors of pregnancy outcomes in patients with lupus: a cohort study. Ann. Intern. Med. 163, 153–163 (2015).
Smyth, A. et al. A systematic review and meta-analysis of pregnancy outcomes in patients with systemic lupus erythematosus and lupus nephritis. Clin. J. Am. Soc. Nephrol. 5, 2060–2068 (2010).
Arkema, E. V. et al. What to expect when expecting with systemic lupus erythematosus (SLE): a population-based study of maternal and fetal outcomes in SLE and pre-SLE. Arthritis Care Res. 68, 988–994 (2016).
Bundhun, P. K., Soogund, M. Z. & Huang, F. Impact of systemic lupus erythematosus on maternal and fetal outcomes following pregnancy: a meta-analysis of studies published between years 2001–2016. J. Autoimmun. 79, 17–27 (2017).
Clowse, M. E. Lupus activity in pregnancy. Rheum. Dis. Clin. North Am. 33, 237–252 (2007).
Bharti, B. et al. Disease severity and pregnancy outcomes in women with rheumatoid arthritis: results from the Organization of Teratology Information Specialists Autoimmune Diseases in Pregnancy Project. J. Rheumatol. 42, 1376–1382 (2015).
Polachek, A., Li, S., Polachek, I. S., Chandran, V. & Gladman, D. Psoriatic arthritis disease activity during pregnancy and the first-year postpartum. Semin. Arthritis Rheum. 46, 740–745 (2017).
Mouyis, M. A., Thornton, C. C., Williams, D. & Giles, I. P. Pregnancy outcomes in patients with psoriatic arthritis. J. Rheumatol. 44, 128–129 (2017).
Gupta, S. & Gupta, N. Sjogren syndrome and pregnancy: a literature review. Perm. J. 21, 16–047 (2017).
Lidar, M. & Langevitz, P. Pregnancy issues in scleroderma. Autoimmun. Rev. 11, A515–A519 (2012).
Jethwa, H., Lam, S., Smith, C. & Giles, I. Does rheumatoid arthritis really improve during pregnancy? A systematic review and metaanalysis. J. Rheumatol. 46, 245–250 (2019).
de Man, Y. A., Dolhain, R. J., van de Geijn, F. E., Willemsen, S. P. & Hazes, J. M. Disease activity of rheumatoid arthritis during pregnancy: results from a nationwide prospective study. Arthritis Rheum. 59, 1241–1248 (2008).
Lockshin, M. D., Reinitz, E., Druzin, M. L., Murrman, M. & Estes, D. Lupus pregnancy. Case-control prospective study demonstrating absence of lupus exacerbation during or after pregnancy. Am. J. Med. 77, 893–898 (1984).
Mintz, G., Niz, J., Gutierrez, G., Garcia-Alonso, A. & Karchmer, S. Prospective study of pregnancy in systemic lupus erythematosus. Results of a multidisciplinary approach. J. Rheumatol. 13, 732–739 (1986).
Wong, K. L., Chan, F. Y. & Lee, C. P. Outcome of pregnancy in patients with systemic lupus erythematosus. A prospective study. Arch. Intern. Med. 151, 269–273 (1991).
Petri, M., Howard, D. & Repke, J. Frequency of lupus flare in pregnancy. The Hopkins Lupus Pregnancy Center experience. Arthritis Rheum. 34, 1538–1545 (1991).
Ruiz-Irastorza, G. et al. Increased rate of lupus flare during pregnancy and the puerperium: a prospective study of 78 pregnancies. Br. J. Rheumatol. 35, 133–138 (1996).
Teng, Y. K. O. et al. An evidence-based approach to pre-pregnancy counselling for patients with systemic lupus erythematosus. Rheumatology 57, 1707–1720 (2018).
Eudy, A. M. et al. Effect of pregnancy on disease flares in patients with systemic lupus erythematosus. Ann. Rheum. Dis. 77, 855–860 (2018).
Ostensen, M. & Husby, G. A prospective clinical study of the effect of pregnancy on rheumatoid arthritis and ankylosing spondylitis. Arthritis Rheum. 26, 1155–1159 (1983).
Ostensen, M. The effect of pregnancy on ankylosing spondylitis, psoriatic arthritis, and juvenile rheumatoid arthritis. Am. J. Reprod. Immunol. 28, 235–237 (1992).
Ostensen, M. Pregnancy in psoriatic arthritis. Scand. J. Rheumatol. 17, 67–70 (1988).
Franceschini, F. & Cavazzana, I. Anti-Ro/SSA and La/SSB antibodies. Autoimmunity 38, 55–63 (2005).
Simister, N. E., Story, C. M., Chen, H. L. & Hunt, J. S. An IgG-transporting Fc receptor expressed in the syncytiotrophoblast of human placenta. Eur. J. Immunol. 26, 1527–1531 (1996).
Costedoat-Chalumeau, N. et al. Outcome of pregnancies in patients with anti-SSA/Ro antibodies: a study of 165 pregnancies, with special focus on electrocardiographic variations in the children and comparison with a control group. Arthritis Rheum. 50, 3187–3194 (2004).
Nield, L. E. et al. Endocardial fibroelastosis associated with maternal anti-Ro and anti-La antibodies in the absence of atrioventricular block. J. Am. Coll. Cardiol. 40, 796–802 (2002).
Zuppa, A. A. et al. Neonatal lupus: follow-up in infants with anti-SSA/Ro antibodies and review of the literature. Autoimmun. Rev. 16, 427–432 (2017).
Miyakis, S. et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J. Thromb. Haemost. 4, 295–306 (2006).
Cervera, R. et al. Morbidity and mortality in the antiphospholipid syndrome during a 10-year period: a multicentre prospective study of 1000 patients. Ann. Rheum. Dis. 74, 1011–1018 (2015).
Alijotas-Reig, J. et al. The European Registry on Obstetric Antiphospholipid Syndrome (EUROAPS): a survey of 247 consecutive cases. Autoimmun. Rev. 14, 387–395 (2015).
Pengo, V. et al. Clinical course of high-risk patients diagnosed with antiphospholipid syndrome. J. Thromb. Haemost. 8, 237–242 (2010).
Ruffatti, A. et al. Antibody profile and clinical course in primary antiphospholipid syndrome with pregnancy morbidity. Thromb. Haemost. 96, 337–341 (2006).
Wahl, D. G. et al. Risk for venous thrombosis related to antiphospholipid antibodies in systemic lupus erythematosus—a meta-analysis. Lupus 6, 467–473 (1997).
Wahl, D. G. et al. Meta-analysis of the risk of venous thrombosis in individuals with antiphospholipid antibodies without underlying autoimmune disease or previous thrombosis. Lupus 7, 15–22 (1998).
Reynaud, Q. et al. Risk of venous and arterial thrombosis according to type of antiphospholipid antibodies in adults without systemic lupus erythematosus: a systematic review and meta-analysis. Autoimmun. Rev. 13, 595–608 (2014).
Alijotas-Reig, J. et al. The European Registry on Obstetric Antiphospholipid Syndrome (EUROAPS): A survey of 1000 consecutive cases. Autoimmun. Rev. 18, 406–414 (2019).
Kallur, S. D., Patil Bada, V., Reddy, P., Pandya, S. & Nirmalan, P. K. Organ dysfunction and organ failure as predictors of outcomes of severe maternal morbidity in an obstetric intensive care unit. J. Clin. Diagn. Res. 8, OC06–OC08 (2014).
Imbasciati, E. et al. Pregnancy in women with pre-existing lupus nephritis: predictors of fetal and maternal outcome. Nephrol. Dial Transplant. 24, 519–525 (2009).
Bramham, K. et al. Pregnancy outcome in women with chronic kidney disease: a prospective cohort study. Reprod. Sci. 18, 623–630 (2011).
Imbasciati, E. et al. Pregnancy in CKD stages 3 to 5: fetal and maternal outcomes. Am. J. Kidney Dis. 49, 753–762 (2007).
Nevis, I. F. et al. Pregnancy outcomes in women with chronic kidney disease: a systematic review. Clin. J. Am. Soc. Nephrol. 6, 2587–2598 (2011).
Jones, D. C. & Hayslett, J. P. Outcome of pregnancy in women with moderate or severe renal insufficiency. N. Engl. J. Med. 335, 226–232 (1996).
Kiely, D. G., Condliffe, R., Wilson, V. J., Gandhi, S. V. & Elliot, C. A. Pregnancy and pulmonary hypertension: a practical approach to management. Obstet. Med. 6, 144–154 (2013).
King, T. E. Jr Restrictive lung disease in pregnancy. Clin. Chest Med. 13, 607–622 (1992).
Anthony, J. & Sliwa, K. Decompensated heart failure in pregnancy. Card. Fail. Rev. 2, 20–26 (2016).
Handler, J. Managing chronic severe hypertension in pregnancy. J. Clin. Hypertens. 8, 738–743 (2006).
Murphy, V. E. et al. Metabolism of synthetic steroids by the human placenta. Placenta 28, 39–46 (2007).
Hwang, J. L. & Weiss, R. E. Steroid-induced diabetes: a clinical and molecular approach to understanding and treatment. Diabetes Metab. Res. Rev. 30, 96–102 (2014).
Smith, C. J. F., Forger, F. & Chambers, C. Predictors for preterm delivery among pregnant women with rheumatoid arthritis and juvenile idiopathic arthritis. Ann. Rheum. Dis. 77, 535 (2018).
Ostensen, M. et al. Anti-inflammatory and immunosuppressive drugs and reproduction. Arthritis Res. Ther. 8, 209 (2006).
Deguchi, M. et al. Factors associated with adverse pregnancy outcomes in women with systematic lupus erythematosus. J. Reprod. Immunol. 125, 39–44 (2018).
Al Arfaj, A. S. & Khalil, N. Pregnancy outcome in 396 pregnancies in patients with SLE in Saudi Arabia. Lupus 19, 1665–1673 (2010).
Clark, C. A., Spitzer, K. A., Nadler, J. N. & Laskin, C. A. Preterm deliveries in women with systemic lupus erythematosus. J. Rheumatol. 30, 2127–2132 (2003).
Kemp, M. W., Newnham, J. P., Challis, J. G., Jobe, A. H. & Stock, S. J. The clinical use of corticosteroids in pregnancy. Hum. Reprod. Update 22, 240–259 (2016).
Brucato, A. et al. Normal neuropsychological development in children with congenital complete heart block who may or may not be exposed to high-dose dexamethasone in utero. Ann. Rheum. Dis. 65, 1422–1426 (2006).
Kelly, E. N., Sananes, R., Chiu-Man, C., Silverman, E. D. & Jaeggi, E. Prenatal anti-Ro antibody exposure, congenital complete atrioventricular heart block, and high-dose steroid therapy impact on neurocognitive outcome in school-age children. Arthritis Rheumatol. 66, 2290–2296 (2014).
Chambers, C. D. et al. Birth outcomes in women who have taken leflunomide during pregnancy. Arthritis Rheum. 62, 1494–1503 (2010).
Coscia, L. A. et al. Update on the teratogenicity of maternal mycophenolate mofetil. J. Pediatr. Genet. 4, 42–55 (2015).
Leroy, C. et al. Immunosuppressive drugs and fertility. Orphanet J. Rare Dis. 10, 136 (2015).
Cassina, M. et al. Pregnancy outcome in women exposed to leflunomide before or during pregnancy. Arthritis Rheum. 64, 2085–2094 (2012).
Weber-Schoendorfer, C., Beck, E., Tissen-Diabate, T. & Schaefer, C. Leflunomide — a human teratogen? A still not answered question. An evaluation of the German Embryotox pharmacovigilance database. Reprod. Toxicol. 71, 101–107 (2017).
Berard, A., Zhao, J. P., Shui, I. & Colilla, S. Leflunomide use during pregnancy and the risk of adverse pregnancy outcomes. Ann. Rheum. Dis. 77, 500–509 (2018).
Keating, G. M. Apremilast: a review in psoriasis and psoriatic arthritis. Drugs 77, 459–472 (2017).
Dhillon, S. Tofacitinib: a review in rheumatoid arthritis. Drugs 77, 1987–2001 (2017).
Al-Salama, Z. T. & Scott, L. J. Baricitinib: a review in rheumatoid arthritis. Drugs 78, 761–772 (2018).
Palmeira, P., Quinello, C., Silveira-Lessa, A. L., Zago, C. A. & Carneiro-Sampaio, M. IgG placental transfer in healthy and pathological pregnancies. Clin. Dev. Immunol. 2012, 985646 (2012).
Nesbitt, A., Kevorkian, L. & Baker, T. Lack of FcRn binding in vitro and no measurable levels of ex vivo placental transfer of certolizumab pegol. Hum. Reprod. 29, 127 (2014).
Herrera-Esparza, R., Bollain-y-Goytia, J. J. & Avalos-Díaz, E. Pathogenic effects of maternal antinuclear antibodies during pregnancy in women with lupus. Rheumatol. Rep. 6, 5545 (2014).
Hyrich, K. L. & Verstappen, S. M. M. Biologic therapies and pregnancy: the story so far. Rheumatology 53, 1377–1385 (2014).
Murashima, A., Watanabe, N., Ozawa, N., Saito, H. & Yamaguchi, K. Etanercept during pregnancy and lactation in a patient with rheumatoid arthritis: drug levels in maternal serum, cord blood, breast milk and the infant’s serum. Ann. Rheumat. Dis. 68, 1793–1794 (2009).
Berthelsen, B. G., Fjeldsoe-Nielsen, H., Nielsen, C. T. & Hellmuth, E. Etanercept concentrations in maternal serum, umbilical cord serum, breast milk and child serum during breastfeeding. Rheumatology 49, 2225–2227 (2010).
Zaretsky, M. V., Alexander, J. M., Byrd, W. & Bawdon, R. E. Transfer of inflammatory cytokines across the placenta. Obstet. Gynecol. 103, 546–550 (2004).
Kumar, M., Ray, L., Vemuri, S. & Simon, T. A. Pregnancy outcomes following exposure to abatacept during pregnancy. Semin. Arthritis Rheum. 45, 351–356 (2015).
Cheent, K. et al. Case report: fatal case of disseminated BCG infection in an infant born to a mother taking infliximab for Crohn’s disease. J. Crohns Colitis 4, 603–605 (2010).
Mariette, X. et al. Lack of placental transfer of certolizumab pegol during pregnancy: results from CRIB, a prospective, postmarketing, pharmacokinetic study. Ann. Rheum. Dis. 77, 228–233 (2018).
Clowse, M. E. et al. Minimal to no transfer of certolizumab pegol into breast milk: results from CRADLE, a prospective, postmarketing, multicentre, pharmacokinetic study. Ann. Rheum. Dis. 76, 1890–1896 (2017).
Hoeltzenbein, M. et al. Tocilizumab use in pregnancy: analysis of a global safety database including data from clinical trials and post-marketing data. Semin. Arthritis Rheum. 46, 238–245 (2016).
Youngstein, T. et al. International multi-centre study of pregnancy outcomes with interleukin-1 inhibitors. Rheumatology 56, 2102–2108 (2017).
Norman, R. J. & Wu, R. The potential danger of COX-2 inhibitors. Fertil. Steril. 81, 493–494 (2004).
National Collaborating Centre for Women’s and Children’s Health (UK). Hypertension in pregnancy: the management of hypertensive disorders during pregnancy. 4: Management of pregnancy with chronic hypertension. NCBI https://www.ncbi.nlm.nih.gov/books/NBK62651/ (2010).
Atallah, A. et al. Aspirin for prevention of preeclampsia. Drugs 77, 1819–1831 (2017).
Asayama, K. & Imai, Y. The impact of salt intake during and after pregnancy. Hypertens. Res. 41, 1–5 (2018).
Podymow, T. & Joseph, G. Preconception and pregnancy management of women with diabetic nephropathy on angiotensin converting enzyme inhibitors. Clin. Nephrol. 83, 73–79 (2015).
Ruiz-Irastorza, G., Khamashta, M. A., Nelson-Piercy, C. & Hughes, G. R. Lupus pregnancy: is heparin a risk factor for osteoporosis? Lupus 10, 597–600 (2001).
Henderson, J. T. et al. Low-dose aspirin for prevention of morbidity and mortality from preeclampsia: a systematic evidence review for the U.S. Preventive Services Task Force. Ann. Intern. Med. 160, 695–703 (2014).
Carlin, A. & Alfirevic, Z. Physiological changes of pregnancy and monitoring. Best Pract. Res. Clin. Obstet. Gynaecol. 22, 801–823 (2008).
Yee, C. S. et al. The BILAG2004-Pregnancy index is reliable for assessment of disease activity in pregnant SLE patients. Rheumatology 51, 1877–1880 (2012).
Bramham, K. et al. Pregnancy outcomes in systemic lupus erythematosus with and without previous nephritis. J. Rheumatol. 38, 1906–1913 (2011).
Espinoza, J. et al. Should bilateral uterine artery notching be used in the risk assessment for preeclampsia, small-for-gestational-age, and gestational hypertension? J. Ultrasound Med. 29, 1103–1115 (2010).
Levine, R. J. et al. Soluble endoglin and other circulating antiangiogenic factors in preeclampsia. N. Engl. J. Med. 355, 992–1005 (2006).
Kim, M. Y. et al. Angiogenic factor imbalance early in pregnancy predicts adverse outcomes in patients with lupus and antiphospholipid antibodies: results of the PROMISSE study. Am J. Obstet. Gynecol. 214, 108.e1–108.e14 (2016).
Kattah, A. G. & Garovic, V. D. The management of hypertension in pregnancy. Adv. Chron. Kidney Dis. 20, 229–239 (2013).
Soh, M. C. & Nelson-Piercy, C. High-risk pregnancy and the rheumatologist. Rheumatology 54, 572–587 (2015).
Orbai, A. M. et al. Anti-C1q antibodies in systemic lupus erythematosus. Lupus 24, 42–49 (2015).
Eudy, A. M. et al. Reasons for cesarean and medically indicated deliveries in pregnancies in women with systemic lupus erythematosus. Lupus 27, 351–356 (2018).
Lee, J. J. & Pope, J. E. A meta-analysis of the risk of venous thromboembolism in inflammatory rheumatic diseases. Arthritis Res. Ther. 16, 435 (2014).
Cohen, H., Arachchillage, D. R., Middeldorp, S., Beyer-Westendorf, J. & Abdul-Kadir, R. Management of direct oral anticoagulants in women of childbearing potential: guidance from the SSC of the ISTH. J. Thromb. Haemost. 14, 1673–1676 (2016).
Izmirly, P. M. et al. Maternal and fetal factors associated with mortality and morbidity in a multi-racial/ethnic registry of anti-SSA/Ro-associated cardiac neonatal lupus. Circulation 124, 1927–1935 (2011).
Clowse, M. E. B. et al. The prevention, screening and treatment of congenital heart block from neonatal lupus: a survey of provider practices. Rheumatology 57, v9–v17 (2018).
Izmirly, P. M. et al. Maternal use of hydroxychloroquine is associated with a reduced risk of recurrent anti-SSA/Ro-antibody-associated cardiac manifestations of neonatal lupus. Circulation 126, 76–82 (2012).
Izmirly, P. M. et al. Evaluation of the risk of anti-SSA/Ro-SSB/La antibody-associated cardiac manifestations of neonatal lupus in fetuses of mothers with systemic lupus erythematosus exposed to hydroxychloroquine. Ann. Rheum. Dis. 69, 1827–1830 (2010).
Martinez-Sanchez, N. et al. Obstetric and perinatal outcome in anti-Ro/SSA-positive pregnant women: a prospective cohort study. Immunol. Res. 65, 487–494 (2017).
Silverman, E. & Jaeggi, E. Non-cardiac manifestations of neonatal lupus erythematosus. Scand. J. Immunol. 72, 223–225 (2010).
Webster, P. et al. Tacrolimus is an effective treatment for lupus nephritis in pregnancy. Lupus 23, 1192–1196 (2014).
Clark, A. L. Clinical uses of intravenous immunoglobulin in pregnancy. Clin. Obstet. Gynecol. 42, 368–380 (1999).
Ruffatti, A. et al. Plasma exchange in the management of high risk pregnant patients with primary antiphospholipid syndrome. A report of 9 cases and a review of the literature. Autoimmun. Rev. 6, 196–202 (2007).
Kurkinen-Raty, M., Koivisto, M. & Jouppila, P. Preterm delivery for maternal or fetal indications: maternal morbidity, neonatal outcome and late sequelae in infants. BJOG 107, 648–655 (2000).
Ostensen, M., Brown, N. D., Chiang, P. K. & Aarbakke, J. Hydroxychloroquine in human breast milk. Eur. J. Clin. Pharmacol. 28, 357 (1985).
Bates, S. M. et al. VTE, thrombophilia, antithrombotic therapy, and pregnancy: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141, e691S–e736S (2012).
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to the research and discussion of the content. I.G. drafted the article and C.-S.Y. and C.G. edited/reviewed the article.
Corresponding author
Ethics declarations
Competing interests
I.G. declares that he has received honoraria and travel grants from UCB and Lupus Academy to speak at educational meetings on topics related to pregnancy in rheumatic disease. C.S.Y. declares that he has consulted for Bristol Myers Squibb, Immupharma and EMD Serono. C.G. declares that she has consulted for and received honoraria from Bristol-Myers Squibb, GlaxoSmithKline, EMD Serono and UCB in relation to lupus clinical trial design and analysis, and has been a member of the speakers’ bureau for GlaxoSmithKline and UCB. C.G. also declares that she has participated in clinical trials sponsored by UCB and funded by Arthritis Research UK with drugs supplied by GlaxoSmithKline.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Glossary
- Intrauterine growth restriction
-
(IUGR). Reduced fetal growth resulting in an estimated weight below the 10th percentile for gestational age.
- Cyclophosphamide-induced gonadal toxicity
-
Gonadal damage induced by cyclophosphamide, leading to reduced ovarian function.
- Gestational hypertension
-
New-onset hypertension presenting after 20 weeks’ gestation without significant proteinuria.
- Pre-eclampsia
-
New-onset hypertension presenting after 20 weeks’ gestation with significant proteinuria. Indicative of maternoplacental dysfunction.
- Small for gestational age
-
Term used to describe a baby who is smaller than usual for the number of weeks of pregnancy. These babies usually have birthweights below the 10th percentile for gestational age.
- Endocardial fibroelastosis
-
A rare heart disorder of infants and children that is characterised by a thickening within the muscular lining of the heart chambers due to an increase in the amount of supporting connective tissue (inelastic collagen) and elastic fibres.
- Placental insufficiency
-
Failure of the placenta to deliver sufficient nutrients and oxygen to the fetus during pregnancy.
- Minimum tolerable dose of corticosteroid
-
The minimum dose required to maintain disease control and reduce complications such as steroid-induced diabetes mellitus, hypertension and infections in the mother.
- Rescue therapy
-
Treatment given after a patient has failed to respond to standard therapy.
- Ductus arteriosus
-
A blood vessel in the fetus connecting the main pulmonary artery to the proximal descending aorta, allowing most blood from the right ventricle to bypass the lungs. Premature closure of this blood vessel leads to progressive right heart dysfunction, congestive heart failure and intrauterine death.
- Uterine artery Doppler ultrasound
-
A technique used to measure uterine artery blood flow between mother and baby.
- Thromboprophylaxis
-
In this context, the prevention of thromboembolic disease by pharmacological means.
- Fetal cardiac ultrasound
-
Technique used to evaluate the structure of the fetal heart.
- Screening for congenital heart block
-
The use of fetal cardiac ultrasound at the 16th to 20th week of pregnancy in anti-SSA/Ro-positive mothers.
- Cardiac pacing
-
Technique used to regulate heart rate involving the fitting of a pacemaker.
Rights and permissions
About this article
Cite this article
Giles, I., Yee, CS. & Gordon, C. Stratifying management of rheumatic disease for pregnancy and breastfeeding. Nat Rev Rheumatol 15, 391–402 (2019). https://doi.org/10.1038/s41584-019-0240-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41584-019-0240-8
This article is cited by
-
Rheumatic Diseases in Reproductive Age—the Possibilities and the Risks
Reproductive Sciences (2023)
-
Systemic sclerosis and pregnancy outcomes: a retrospective study from a single center
Arthritis Research & Therapy (2022)
-
Leflunomide Exposure and Teriflunomide Concentrations up to the Third Trimester of Pregnancy: A Case Report
Clinical Drug Investigation (2022)
-
Risk factors for adverse pregnancy outcomes in women with rheumatoid arthritis and follow-up of their offspring
Clinical Rheumatology (2022)
-
Association of various myositis-specific autoantibodies with dermatomyositis and polymyositis triggered by pregnancy
Rheumatology International (2022)