Abstract
Objective
Gastric cancer is one of the most common causes of cancer-related death worldwide. Medicinal plants are one of the main sources for discovery of new pharmacological agents especially for treatment of cancers. The aim of the present study is to review pharmacotherapeutic aspects of three mostly studied phytochemicals including curcumin, quercetin, and allicin for management of gastric cancer.
Methods
Scopus, PubMed, Web of Science, and Google Scholar were searched for the effects of curcumin, quercetin, allicin, and their analogs in gastric cancer. Data were collected up to November 2015. The search terms were “curcumin,” “quercetin,” “allicin,” and “gastric cancer” or “cancer.”
Results
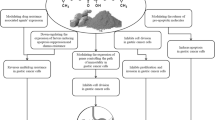
Curcumin demonstrated anti-angiogenic, anti-proliferative, anti-metastatic, pro-apoptotic, and anti-helicobacter activities. Quercetin inhibited cell growth and induced apoptosis, necrosis, and autophagy as well as anti-Helicobacter activity. Allicin showed apoptotic and anti-Helicobacter properties. All three natural compounds had low bioavailability.
Conclusions
Although preclinical studies demonstrated the activity of curcumin, quercetin, and allicin in gastric cancer, clinical trials are needed to confirm their effectiveness. Applying their possible synergistic action and suitable drug delivery system in clinical studies can be also an attractive approach with the purpose of finding new extremely efficient anti-gastric cancer agents.
Mini-Abstract
Curcumin, quercetin, and allicin seem to be good candidates for management of gastric cancer through their pro-apoptotic, anti-proliferative, and anti-helicobacter activities.



Similar content being viewed by others
References
Wadhwa R, Song S, Lee J-S, et al. Gastric cancer—molecular and clinical dimensions. Nat Rev Clin Oncol. 2013;10:643–55.
McLean MH, El-Omar EM. Genetics of gastric cancer. Nat Rev Gastroenterol Hepatol. 2014;
Romano M, Ricci V, Zarrilli R. Mechanisms of disease: Helicobacter pylori-related gastric carcinogenesis—implications for chemoprevention. Nat Clin Pract Gastroenterol Hepatol. 2006;3:622–32.
Peek RM, Blaser MJ. Helicobacter pylori and gastrointestinal tract adenocarcinomas. Nat Rev Cancer. 2002;2:28–37.
Tsai H-F, Hsu P-N. Interplay between Helicobacter pylori and immune cells in immune pathogenesis of gastric inflammation and mucosal pathology. Cell Mol Immunol. 2010;7:255–9.
Wroblewski LE, Peek RM, Wilson KT. Helicobacter pylori and gastric cancer: factors that modulate disease risk. Clin Microbiol Rev. 2010;23:713–39.
Crawford HC, Krishna US, Israel DA, et al. Helicobacter pylori strain-selective induction of matrix metalloproteinase-7 in vitro and within gastric mucosa. Gastroenterology. 2003;125:1125–36.
Lee SY, Shin YW, Hahm KB. Phytoceuticals: mighty but ignored weapons against Helicobacter pylori infection. J Dig Dis. 2008;9:129–39.
Gupta SC, Patchva S, Aggarwal BB. Therapeutic roles of curcumin: lessons learned from clinical trials. AAPS J. 2013;15:195–218.
Boughan PK, Argent RH, Body-Malapel M, et al. Nucleotide-binding oligomerization domain-1 and epidermal growth factor receptor critical regulators of β-defensins during Helicobacter pylori infection. J Biol Chem. 2006;281:11637–48.
Yan F, Cao H, Chaturvedi R, et al. Epidermal growth factor receptor activation protects gastric epithelial cells from Helicobacter pylori-induced apoptosis. Gastroenterology. 2009;136:1297–307. e3.
Wong BC, Zhang L, Ma J-l, et al. Effects of selective COX-2 inhibitor and Helicobacter pylori eradication on precancerous gastric lesions. Gut 2011:gutjnl-2011-300154.
Wu C-Y, Wang C-J, Tseng C-C, et al. Helicobacter pylori promote gastric cancer cells invasion through a NF-kappaB and COX-2-mediated pathway. World J Gastroenterol. 2005;11:3197.
Keates S, Keates AC, Katchar K, et al. Helicobacter pylori induces up-regulation of the epidermal growth factor receptor in AGS gastric epithelial cells. J Infect Dis. 2007;196:95–103.
Li J, Shen L, Lu F-r, et al. Plumbagin inhibits cell growth and potentiates apoptosis in human gastric cancer cells in vitro through the NF-κB signaling pathway. Acta Pharmacol Sin. 2012;33:242–9.
Yu L-L, Wu J-G, Dai N, et al. Curcumin reverses chemoresistance of human gastric cancer cells by downregulating the NF-κB transcription factor. Oncol Rep. 2011;26:1197.
Dorai T, Aggarwal BB. Role of chemopreventive agents in cancer therapy. Cancer Lett. 2004;215:129–40.
Karin M, Cao Y, Greten FR, et al. NF-κB in cancer: from innocent bystander to major culprit. Nat Rev Cancer. 2002;2:301–10.
Ema A, Yamashita K, Sakuramoto S, et al. Lymph node ratio is a critical prognostic predictor in gastric cancer treated with S-1 chemotherapy. Gastric Cancer. 2014;17:67–75.
Sarkar FH, Li Y, Wang Z, et al. Lesson learned from nature for the development of novel anti-cancer agents: implication of isoflavone, curcumin, and their synthetic analogs. Curr Pharm Des. 2010;16:1801.
Aqil F, Munagala R, Jeyabalan J, et al. Bioavailability of phytochemicals and its enhancement by drug delivery systems. Cancer Lett. 2013;334:133–41.
Koosirirat C, Linpisarn S, Changsom D, et al. Investigation of the anti-inflammatory effect of Curcuma longa in Helicobacter pylori-infected patients. Int Immunopharmacol. 2010;10:815–8.
Peng Y-m, Zheng J-b, Zhou Y-b, et al. Characterization of a novel curcumin analog P1 as potent inhibitor of the NF-κB signaling pathway with distinct mechanisms. Acta Pharmacol Sin. 2013;34:939–50.
Shehzad A, Wahid F, Lee YS. Curcumin in cancer chemoprevention: molecular targets, pharmacokinetics, bioavailability, and clinical trials. Arch Pharm. 2010;343:489–99.
Duvoix A, Blasius R, Delhalle S, et al. Chemopreventive and therapeutic effects of curcumin. Cancer Lett. 2005;223:181–90.
Kunnumakkara AB, Guha S, Krishnan S, et al. Curcumin potentiates antitumor activity of gemcitabine in an orthotopic model of pancreatic cancer through suppression of proliferation, angiogenesis, and inhibition of nuclear factor-κB–regulated gene products. Cancer Res. 2007;67:3853–61.
Foryst-Ludwig A, Neumann M, Schneider-Brachert W, et al. Curcumin blocks NF-κB and the motogenic response in Helicobacter pylori-infected epithelial cells. Biochem Biophys Res Commun. 2004;316:1065–72.
Woo J-H, Kim Y-H, Choi Y-J, et al. Molecular mechanisms of curcumin-induced cytotoxicity: induction of apoptosis through generation of reactive oxygen species, down-regulation of Bcl-XL and IAP, the release of cytochrome c and inhibition of Akt. Carcinogenesis. 2003;24:1199–208.
Shehzad A, Khan S, Shehzad O, et al. Curcumin therapeutic promises and bioavailability in colorectal cancer. Drugs of Today. 2010;46:523.
Kuttan G, Kumar KBH, Guruvayoorappan C, et al. Antitumor, anti-invasion, and antimetastatic effects of curcumin. The molecular targets and therapeutic uses of curcumin in health and disease. Springer; 2007. p. 173–84.
Amagase H. Clarifying the real bioactive constituents of garlic. J Nutr. 2006;136:716S–25S.
Xue X, Yu J-L, Sun D-Q, et al. Curcumin induces apoptosis in SGC-7901 gastric adenocarcinoma cells via regulation of mitochondrial signaling pathways. Asian Pac J Cancer Prev. 2014;15:3987–92.
Cai X-Z, Wang J, Xiao-Dong L, et al. Curcumin suppresses proliferation and invasion in human gastric cancer cells by down-regulation of PAK1 activity and cyclin D1 expression. Cancer Biol Ther. 2009;8:1360–8.
Cao A-L, Tang Q-F, Zhou W-C, et al. Ras/ERK signaling pathway is involved in curcumin-induced cell cycle arrest and apoptosis in human gastric carcinoma AGS cells. J Asian Nat Prod Res 2014:1–8.
Shehzad A, Lee J, Lee YS. Curcumin in various cancers. Biofactors. 2013;39:56–68.
Singletary K, Milner J. Diet, autophagy, and cancer: a review. Cancer Epidemiol Biomark Prev. 2008;17:1596–610.
Lee YJ, Kim N-Y, Suh Y-A, et al. Involvement of ROS in curcumin-induced autophagic cell death. Korean J Physiol Pharmacol. 2011;15:1–7.
Zhang S-F, Wang X-L, Yang X-Q, et al. Autophagy-associated targeting pathways of natural products during cancer treatment. Asian Pac J Cancer Prev: APJCP. 2014;15:10557.
Sintara K, Thong-Ngam D, Patumraj S, et al. Curcumin suppresses gastric NF-κB activation and macromolecular leakage in Helicobacter pylori-infected rats. World J Gastroenterol: WJG. 2010;16:4039.
Shaikh J, Ankola D, Beniwal V, et al. Nanoparticle encapsulation improves oral bioavailability of curcumin by at least 9-fold when compared to curcumin administered with piperine as absorption enhancer. Eur J Pharm Sci. 2009;37:223–30.
Anand P, Kunnumakkara AB, Newman RA, et al. Bioavailability of curcumin: problems and promises. Mol Pharm. 2007;4:807–18.
Zhang L, Kong Y, Wu D, et al. Three flavonoids targeting the β-hydroxyacyl-acyl carrier protein dehydratase from Helicobacter pylori: crystal structure characterization with enzymatic inhibition assay. Protein Sci. 2008;17:1971–8.
Dajas F. Life or death: neuroprotective and anticancer effects of quercetin. J Ethnopharmacol. 2012;143:383–96.
Chen C, Zhou J, Ji C. Quercetin: a potential drug to reverse multidrug resistance. Life Sci. 2010;87:333–8.
Dutta KR, Banerjee S, Mitra A. Medicinal plants of West Midnapore, India: emphasis on phytochemical containment having role on oral cancer. Int J Phytopharmacol. 2012;3:198–208.
Bi Y, Shen C, Li C, et al. Inhibition of autophagy induced by quercetin at a late stage enhances cytotoxic effects on glioma cells. Tumor Biol. 2015:1–12.
Jeong JH, An JY, Kwon YT, et al. Effects of low dose quercetin: cancer cell-specific inhibition of cell cycle progression. J Cell Biochem. 2009;106:73–82.
Hu X-T, Ding C, Zhou N, et al. Quercetin protects gastric epithelial cell from oxidative damage in vitro and in vivo. Eur J Pharmacol. 2015;
Bishayee K, Ghosh S, Mukherjee A, et al. Quercetin induces cytochrome-c release and ROS accumulation to promote apoptosis and arrest the cell cycle in G2/M, in cervical carcinoma: signal cascade and drug-DNA interaction. Cell Prolif. 2013;46:153–63.
Borska S, Chmielewska M, Wysocka T, et al. In vitro effect of quercetin on human gastric carcinoma: targeting cancer cells death and MDR. Food Chem Toxicol. 2012;50:3375–83.
Gibellini L, Pinti M, Nasi M, et al. Quercetin and cancer chemoprevention. Evidence-based complementary and alternative medicine 2011;2011.
Ekström A, Serafini M, Nyren O, et al. Dietary quercetin intake and risk of gastric cancer: results from a population-based study in Sweden. Ann Oncol. 2011;22:438–43.
Nguyen T, Tran E, Nguyen T, et al. The role of activated MEK-ERK pathway in quercetin-induced growth inhibition and apoptosis in A549 lung cancer cells. Carcinogenesis. 2004;25:647–59.
Rivera AR, Castillo-Pichardo L, Gerena Y, et al. Anti-breast cancer potential of quercetin via the Akt/AMPK/mammalian target of rapamycin (mTOR) signaling cascade. PLoS One. 2016;11:e0157251.
Ranelletti FO, Ricci R, Larocca LM, et al. Growth-inhibitory effect of quercetin and presence of type-II estrogen-binding sites in human colon-cancer cell lines and primary colorectal tumors. Int J Cancer. 1992;50:486–92.
Shen X, Si Y, Wang Z, et al. Quercetin inhibits the growth of human gastric cancer stem cells by inducing mitochondrial-dependent apoptosis through the inhibition of PI3K/Akt signaling. Int J Mol Med. 2016;
Wang P, Zhang K, Zhang Q, et al. Effects of quercetin on the apoptosis of the human gastric carcinoma cells. Toxicol in Vitro. 2012;26:221–8.
González-Segovia R, Quintanar JL, Salinas E, et al. Effect of the flavonoid quercetin on inflammation and lipid peroxidation induced by Helicobacter pylori in gastric mucosa of guinea pig. J Gastroenterol. 2008;43:441–7.
Psahoulia FH, Moumtzi S, Roberts ML, et al. Quercetin mediates preferential degradation of oncogenic Ras and causes autophagy in Ha-RAS-transformed human colon cells. Carcinogenesis. 2007;28:1021–31.
Wang K, Liu R, Li J, et al. Quercetin induces protective autophagy in gastric cancer cells: involvement of Akt-mTOR-and hypoxia-induced factor 1α-mediated signaling. Autophagy. 2011;7:966–78.
Wiczkowski W, Romaszko J, Bucinski A, et al. Quercetin from shallots (Allium cepa L. var. aggregatum) is more bioavailable than its glucosides. J Nutr. 2008;138:885–8.
Chakraborty S, Stalin S, Das N, et al. The use of nano-quercetin to arrest mitochondrial damage and MMP-9 upregulation during prevention of gastric inflammation induced by ethanol in rat. Biomaterials. 2012;33:2991–3001.
Bat-Chen W, Golan T, Peri I, et al. Allicin purified from fresh garlic cloves induces apoptosis in colon cancer cells via Nrf2. Nutr Cancer. 2010;62:947–57.
Borlinghaus J, Albrecht F, Gruhlke MC, et al. Allicin: chemistry and biological properties. Molecules. 2014;19:12591–618.
Zhang Z-m, Zhong N, Gao H-q, et al. Inducing apoptosis and upregulation of Bax and Fas ligand expression by allicin in hepatocellular carcinoma in Balb/c nude mice. Chin Med J-Beijing-Engl Ed. 2006;119:422.
Cha JH, Choi YJ, Cha SH, et al. Allicin inhibits cell growth and induces apoptosis in U87MG human glioblastoma cells through an ERK-dependent pathway. Oncol Rep. 2012;28:41–8.
Park B, Kim K, Rhee D-K, et al. The apoptotic effect of allicin in MCF-7 human breast cancer cells: role for ATF3. The FASEB J. 2012;2012
Park S-Y, Cho S-J, H-c K, et al. Caspase-independent cell death by allicin in human epithelial carcinoma cells: involvement of PKA. Cancer Lett. 2005;224:123–32.
Tao M, Gao L, Pan J, et al. Study on the inhibitory effect of allicin on human gastric cancer cell line sgc-7901 and its mechanism. Afr J Tradit Complement Altern Med. 2013;11:176–9.
Yang JY, Della-Fera MA, Nelson-Dooley C, et al. Molecular mechanisms of apoptosis induced by ajoene in 3T3-L1 adipocytes. Obesity. 2006;14:388–97.
Chu Y-L, Ho C-T, Chung J-G, et al. Allicin induces p53-mediated autophagy in Hep G2 human liver cancer cells. J Agric Food Chem. 2012;60:8363–71.
Sun L, Wang X. Effects of allicin on both telomerase activity and apoptosis in gastric cancer SGC-7901 cells. World J Gastroenterol. 2003;9:1930–4.
Sivam GP. Protection against Helicobacter pylori and other bacterial infections by garlic. J Nutr. 2001;131:1106S–8S.
O'Gara EA, Hill DJ, Maslin DJ. Activities of garlic oil, garlic powder, and their diallyl constituents against Helicobacter pylori. Appl Environ Microbiol. 2000;66:2269–73.
Takeuchi H, Trang VT, Morimoto N, et al. Natural products and food components with anti-Helicobacter pylori activities. World J Gastroenterol: WJG. 2014;20:8971.
Nicastro HL, Ross SA, Milner JA. Garlic and onions: their cancer prevention properties. Cancer Prev Res 2015:canprevres. 0172.2014.
Vazquez-Prieto MA, Miatello RM. Organosulfur compounds and cardiovascular disease. Mol Asp Med. 2010;31:540–5.
Alpers DH. Garlic and its potential for prevention of colorectal cancer and other conditions. Curr Opin Gastroenterol. 2009;25:116–21.
Iciek M, Kwiecień I, Włodek L. Biological properties of garlic and garlic-derived organosulfur compounds. Environ Mol Mutagen. 2009;50:247–65.
Lu Q, Lu P-M, Piao J-H, et al. Preparation and physicochemical characteristics of an allicin nanoliposome and its release behavior. LWT-Food Sci Technol. 2014;57:686–95.
Arbiser JL, Klauber N, Rohan R, et al. Curcumin is an in vivo inhibitor of angiogenesis. Mol Med. 1998;4:376.
Kunnumakkara AB, Anand P, Aggarwal BB. Curcumin inhibits proliferation, invasion, angiogenesis and metastasis of different cancers through interaction with multiple cell signaling proteins. Cancer Lett. 2008;269:199–225.
Dolcet X, Llobet D, Pallares J, et al. NF-kB in development and progression of human cancer. Virchows Arch. 2005;446:475–82.
Moon J-H, Eo SK, Lee JH, et al. Quercetin-induced autophagy flux enhances TRAIL-mediated tumor cell death. Oncol Rep. 2015;34:375–81.
Lawson LD, Wang ZJ. Low allicin release from garlic supplements: a major problem due to the sensitivities of alliinase activity. J Agric Food Chem. 2001;49:2592–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Haghi, A., Azimi, H. & Rahimi, R. A Comprehensive Review on Pharmacotherapeutics of Three Phytochemicals, Curcumin, Quercetin, and Allicin, in the Treatment of Gastric Cancer. J Gastrointest Canc 48, 314–320 (2017). https://doi.org/10.1007/s12029-017-9997-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-017-9997-7