Abstract
Aim
To assess the performance of HbA1c and the 1-h plasma glucose (PG ≥ 155 mg/dl; 8.6 mmol/l) in identifying dysglycemia based on the oral glucose tolerance test (OGTT) from a real-world clinical care setting.
Methods
This was a diagnostic test accuracy study. For this analysis, we tested the HbA1c diagnostic criteria advocated by the American Diabetes Association (ADA 5.7–6.4 %) and International Expert Committee (IEC 6.0–6.4 %) against conventional OGTT criteria. We also tested the utility of 1-h PG ≥ mg/dl; 8.6 mmol/l. Prediabetes was defined according to ADA-OGTT guidelines. Spearman correlation tests were used to determine the relationships between HbA1c, 1-h PG with fasting, 2-h PG and indices of insulin sensitivity and β-cell function. The levels of agreement between diagnostic methods were ascertained using Cohen’s kappa coefficient (Κ). Receiver operating characteristic (ROC) curve was used to analyze the performance of the HbA1c and 1-h PG test in identifying prediabetes considering OGTT as reference diagnostic criteria. The diagnostic properties of different HbA1c thresholds were contrasted by determining sensitivity, specificity and likelihood ratios (LR).
Results
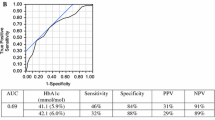
Of the 212 high-risk individuals, 70 (33 %) were identified with prediabetes, and 1-h PG showed a stronger association with 2-h PG, insulin sensitivity index, and β-cell function than HbA1c (P < 0.05). Furthermore, the level of agreement between 1-h PG ≥ 155 mg/dl (8.6 mmol/l) and the OGTT (Κ[95 % CI]: 0.40[0.28–0.53]) diagnostic test was stronger than that of ADA-HbA1c criteria 0.1[0.03–0.16] and IEC criteria (0.17[0.04–0.30]). The ROC (AUC[95 % CI]) for HbA1c and 1-h PG were 0.65[0.57–0.73] and 0.79[0.72–0.85], respectively. Importantly, 1-h PG ≥ 155 mg/dl (8.6 mmol/l) showed good sensitivity (74.3 % [62.4–84.0]) and specificity 69.7 % [61.5–77.1]) with a LR of 2.45. The ability of 1-h PG to discriminate prediabetes was better than that of HbA1c (∆AUC: −0.14; Z value: 2.5683; P = 0.01022).
Conclusion
In a real-world clinical practice setting, the 1-h PG ≥ 155 mg/dl (8.6 mmol/l) is superior for detecting high-risk individuals compared with HbA1c. Furthermore, HbA1c is a less precise correlate of insulin sensitivity and β-cell function than the 1-h PG and correlates poorly with the 2-h PG during the OGTT.



Similar content being viewed by others
References
Gregg EW, Zhuo X, Cheng YJ, Albright AL, Narayan KMV, Thompson TJ (2014) Trends in lifetime risk and years of life lost due to diabetes in the USA, 1985–2011: a modelling study. Lancet Diabetes Endocrinol 2(11):867–874. doi:10.1016/S2213-8587(14)70161-5
Centers for Disease Control and Prevention (CDC) Awareness of prediabetes–United States, 2005–2010 (2013). MMWR Morbidity and mortality weekly report 62 (11):209–212
Barhak J, Isaman DJM, Ye W, Lee D (2010) Chronic disease modeling and simulation software. J Biomed Inform 43(5):791–799. doi:10.1016/j.jbi.2010.06.003
Herman WH, Ye W, Griffin SJ et al (2015) Early detection and treatment of type 2 diabetes reduce cardiovascular morbidity and mortality: a simulation of the results of the Anglo-Danish-Dutch study of intensive treatment in people with screen-detected diabetes in primary care (ADDITION-Europe). Diabetes Care: dc142459
Meier JJ, Bonadonna RC (2013) Role of reduced β-cell mass versus impaired β-cell function in the pathogenesis of type 2 diabetes. Diabetes Care 36(Suppl 2):S113–S119. doi:10.2337/dcS13-2008
Nichols GA, Alexander CM, Girman CJ, Kamal-Bahl SJ, Brown JB (2006) Treatment escalation and rise in HbA1c following successful initial metformin therapy. Diabetes Care 29(3):504–509
Haffner SM, Stern MP, Hazuda HP, Mitchell BD, Patterson JK (1990) Cardiovascular risk factors in confirmed prediabetic individuals: Does the clock for coronary heart disease start ticking before the onset of clinical diabetes? JAMA 263(21):2893–2898
Bergman M (2014) The early diabetes intervention program–Is early actually late? Diabetes/Metab Res Rev 30(8):654–658. doi:10.1002/dmrr.2563
Nathan DM, Davidson MB, DeFronzo RA et al (2007) Impaired fasting glucose and impaired glucose tolerance: implications for care. Diabetes Care 30(3):753–759. doi:10.2337/dc07-9920
Gohdes D, Amundson H, Oser CS, Helgerson SD, Harwell TS (2009) How are we diagnosing cardiometabolic risk in primary care settings? Primary Care Diabetes 3(1):29–35. doi:10.1016/j.pcd.2008.12.002
Committee IE (2009) International Expert Committee report on the role of the A1C assay in the diagnosis of diabetes. Diabetes Care 32(7):1327–1334
Association AD (2010) Diagnosis and classification of diabetes mellitus. Diabetes Care 33(Supplement 1):S62–S69
Rathmann W, Kowall B, Tamayo T et al (2012) Hemoglobin A1c and glucose criteria identify different subjects as having type 2 diabetes in middle-aged and older populations: the KORA S4/F4 Study. Ann Med 44(2):170–177. doi:10.3109/07853890.2010.531759
Olson DE, Rhee MK, Herrick K, Ziemer DC, Twombly JG, Phillips LS (2010) Screening for diabetes and pre-diabetes with proposed A1C-based diagnostic criteria. Diabetes Care 33(10):2184–2189. doi:10.2337/dc10-0433
Cosson E, Chiheb S, Cussac-Pillegand C et al (2013) Haemoglobin glycation may partly explain the discordance between HbA1c measurement and oral glucose tolerance test to diagnose dysglycaemia in overweight/obese subjects. Diabetes Metab 39(2):118–125. doi:10.1016/j.diabet.2012.08.013
Marini MA, Succurro E, Frontoni S et al (2012) Insulin sensitivity, beta-cell function, and incretin effect in individuals with elevated 1-hour postload plasma glucose levels. Diabetes Care 35(4):868–872. doi:10.2337/dc11-2181
Bonora E, Tuomilehto J (2011) The pros and cons of diagnosing diabetes with A1C. Diabetes Care 34(Suppl 2):S184–S190. doi:10.2337/dc11-s216
Bergman M, Chetrit A, Roth J, Dankner R (2015) Dysglycemia and long-term mortality: observations from the Israel study of glucose intolerance, obesity and hypertension. Diabetes/Metab Res Rev 31(4):368–375. doi:10.1002/dmrr.2618
Jagannathan R, Sevick MA, Li H et al (2015) Elevated 1-hour plasma glucose levels are associated with dysglycemia, impaired beta-cell function, and insulin sensitivity: a pilot study from a real world health care setting. Endocrine. doi:10.1007/s12020-015-0746-z
Abdul-Ghani MA, Lyssenko V, Tuomi T, DeFronzo RA, Groop L (2009) Fasting versus postload plasma glucose concentration and the risk for future type 2 diabetes: results from the Botnia Study. Diabetes Care 32(2):281–286. doi:10.2337/dc08-1264
Alyass A, Almgren P, Akerlund M et al (2015) Modelling of OGTT curve identifies 1 h plasma glucose level as a strong predictor of incident type 2 diabetes: results from two prospective cohorts. Diabetologia 58(1):87–97. doi:10.1007/s00125-014-3390-x
Sesti G, Hribal ML, Fiorentino TV, Sciacqua A, Perticone F (2014) Elevated 1 h postload plasma glucose levels identify adults with normal glucose tolerance but increased risk of non-alcoholic fatty liver disease. BMJ Open Diabetes Res Care 2(1):e000016. doi:10.1136/bmjdrc-2014-000016
Bardini G, Dicembrini I, Cresci B, Rotella CM (2010) Inflammation markers and metabolic characteristics of subjects with 1-h plasma glucose levels. Diabetes Care 33(2):411–413. doi:10.2337/dc09-1342
Succurro E, Marini MA, Arturi F et al (2009) Elevated one-hour post-load plasma glucose levels identifies subjects with normal glucose tolerance but early carotid atherosclerosis. Atherosclerosis 207(1):245–249. doi:10.1016/j.atherosclerosis.2009.04.006
Temelkova-Kurktschiev TS, Koehler C, Henkel E, Leonhardt W, Fuecker K, Hanefeld M (2000) Postchallenge plasma glucose and glycemic spikes are more strongly associated with atherosclerosis than fasting glucose or HbA1c level. Diabetes Care 23(12):1830–1834
Succurro E, Arturi F, Lugara M et al (2010) One-hour postload plasma glucose levels are associated with kidney dysfunction. Clin J Am Soc Nephrol CJASN 5(11):1922–1927. doi:10.2215/CJN.03240410
Bianchi C, Miccoli R, Trombetta M et al (2013) Elevated 1-hour postload plasma glucose levels identify subjects with normal glucose tolerance but impaired beta-cell function, insulin resistance, and worse cardiovascular risk profile: the GENFIEV study. Journal Clin Endocrinol Metab 98(5):2100–2105. doi:10.1210/jc.2012-3971
Bossuyt PM, Reitsma JB, Bruns DE et al (2003) Towards complete and accurate reporting of studies of diagnostic accuracy: the STARD initiative: standards for reporting of diagnostic accuracy. Clin Chem 49(1):1–6
Matsuda M, DeFronzo RA (1999) Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes Care 22(9):1462–1470
Ram J, Snehalatha C, Selvam S et al (2015) The oral disposition index is a strong predictor of incident diabetes in Asian Indian prediabetic men. Acta Diabetol. doi:10.1007/s00592-015-0718-z
Kanat M, Winnier D, Norton L et al (2011) The relationship between {beta}-cell function and glycated hemoglobin: results from the veterans administration genetic epidemiology study. Diabetes Care 34(4):1006–1010. doi:10.2337/dc10-1352
Li C, Yang H, Tong G, et al (2014) Correlations between A1c, fasting glucose, 2 h postload glucose, and β-cell function in the Chinese population. Acta Diabetol 51(4):601–608
Fiorentino TV, Marini MA, Andreozzi F et al (2015) One-hour postload hyperglycemia is a stronger predictor of type 2 diabetes than impaired fasting glucose. J Clin Endocrinol Metab 100(10):3744–3751
Fizelova M, Stancakova A, Lorenzo C et al (2015) Glycated hemoglobin levels are mostly dependent on nonglycemic parameters in 9398 Finnish men without diabetes. J Clin Endocrinol Metab 100(5):1989–1996. doi:10.1210/jc.2014-4121
Oka R, Aizawa T, Miyamoto S, Yoneda T, Yamagishi M (2015) One-hour plasma glucose as a predictor of the development of Type 2 diabetes in Japanese adults. Diabetic Med J Br Diabetic Assoc. doi:10.1111/dme.12994
Kahn R, Davidson MB (2014) The reality of type 2 diabetes prevention. Diabetes Care 37(4):943–949. doi:10.2337/dc13-1954
Christensen DL, Witte DR, Kaduka L et al (2010) Moving to an A1C-based diagnosis of diabetes has a different impact on prevalence in different ethnic groups. Diabetes Care 33(3):580–582
Silverman RA, Thakker U, Ellman T et al (2011) Hemoglobin A1c as a screen for previously undiagnosed prediabetes and diabetes in an acute-care setting. Diabetes Care 34(9):1908–1912. doi:10.2337/dc10-0996
Mohan V, Vijayachandrika V, Gokulakrishnan K et al (2010) A1C cut points to define various glucose intolerance groups in Asian Indians. Diabetes Care 33(3):515–519. doi:10.2337/dc09-1694
Manco M, Panunzi S, Macfarlane DP et al (2010) Relationship between Insulin S, Cardiovascular Risk C, One-hour plasma glucose identifies insulin resistance and beta-cell dysfunction in individuals with normal glucose tolerance: cross-sectional data from the Relationship between Insulin Sensitivity and Cardiovascular Risk (RISC) study. Diabetes Care 33(9):2090–2097. doi:10.2337/dc09-2261
Priya M, Anjana RM, Chiwanga FS, Gokulakrishnan K, Deepa M, Mohan V (2013) 1-hour venous plasma glucose and incident prediabetes and diabetes in Asian indians. Diabetes Technol Ther 15(6):497–502. doi:10.1089/dia.2013.0025
Acknowledgments
This study was funded by CTSI Grant Number 1UL1RR029893 (NCRR, NIH, and the Schuman Foundation) and partly by NIH-K24-NR012226.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
This study was approved by the New York University School of Medicine Institutional Review Board.
Human and animal rights disclosure
All human rights were observed in keeping with Declaration of Helsinki 2008 (ICH GCP). There are no animal rights issues as this is a clinical study.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Managed by Antonio Secchi.
Rights and permissions
About this article
Cite this article
Jagannathan, R., Sevick, M.A., Fink, D. et al. The 1-hour post-load glucose level is more effective than HbA1c for screening dysglycemia. Acta Diabetol 53, 543–550 (2016). https://doi.org/10.1007/s00592-015-0829-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-015-0829-6