Abstract
Background
The aim was to determine the patients’ characteristics, comorbidity, and inpatient treatment features of very old otorhinolaryngology patients (80+ years) compared to old patients (75–79 years).
Methods
A single-center cohort study in a tertiary and university care center was performed with 144 old and 143 very old patients who were hospitalized in 2012. Predictors for differences between old and very old patients were analyzed univariately and multivariately using regression models.
Results
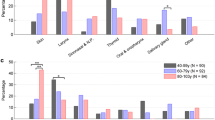
Ear (30 %) and nose/paranasal sinus (23 %) diseases were the most frequent reasons for hospitalization. Baseline and disease characteristics were not different between the two groups of elderly patients. Duration of hospitalization was no longer in very old patients (p = 0.827). Mobility (p = 0.017), dietary intake (p = 0.017), and having hearing aid (p < 0.0001) were independent comorbidity predictors in very old patients compared to old patients. Polymedication was found less frequently in very old patients (p = 0.017). To take cardiovascular drugs (p = 0.009) or psychotherapeutic drugs (p = 0.045) were independent permanent medication predictors in very old patients compared to old patients. About half of the patients received a surgical treatment (52 %) and the other half a conservative treatment (48 %). The very old patients received significantly more often an antibiotic treatment (p < 0.0001). Complication rates for surgical cases and non-surgical cases were not different (p = 0.686 and p = 0.524, respectively).
Conclusions
Although comorbidity continues to increase in hospitalized very old compared to old otorhinolaryngology patients, most of the disease, treatment and treatment related complication characteristics seem not to change significantly from old to very old patients.

Similar content being viewed by others
References
Creighton FX Jr, Poliashenko SM, Statham MM, Abramson P, Johns MM 3rd (2013) The growing geriatric otolaryngology patient population: a study of 131,700 new patient encounters. Laryngoscope 123:97–102
Io Medicine (2008) Retooling for an aging America: building the healthcare workforce. The National Academies Press, Washington, DC
Lin HW, Bhattacharyya N (2011) Otologic diagnoses in the elderly: current utilization and predicted workload increase. Laryngoscope 121:1504–1507
Genther DJ, Gourin CG (2015) Effect of comorbidity on short-term outcomes and cost of care after head and neck cancer surgery in the elderly. Head Neck 37:685–693
Genther DJ, Frick KD, Chen D, Betz J, Lin FR (2013) Association of hearing loss with hospitalization and burden of disease in older adults. JAMA 309:2322–2324
D’Hoore W, Sicotte C, Tilquin C (1993) Risk adjustment in outcome assessment: the Charlson comorbidity index. Methods Inf Med 32:382–387
Bhattacharyya N (2011) The increasing workload in head and neck surgery: an epidemiologic analysis. Laryngoscope 121:111–115
Wu JM, Matthews CA, Vaughan CP, Markland AD (2015) Urinary, fecal, and dual incontinence in older US adults. J Am Ger Soc 63:947–953
Stoddart H, Donovan J, Whitley E, Sharp D, Harvey I (2001) Urinary incontinence in older people in the community: a neglected problem? Br J Gen Pract 51:548–552
Schachtele S, Tumena T, Gassmann KG, Fromm MF, Maas R (2014) Implementation of warnings from Dear Doctor Letters (Rote-Hand-Briefe): an analysis of medication data from a large cohort of elderly patients. Dtsch Arztebl Int 111:255–263
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatry Res 12:189–198
Smith R (1994) Validation and reliability of the elderly mobility scale. Physiotherapy 80:744–747
Sundararajan V, Henderson T, Perry C, Muggivan A, Quan H, Ghali WA (2004) New ICD-10 version of the Charlson comorbidity index predicted in-hospital mortality. J Clin Epidemiol 57:1288–1294
Kirkhus L, Jordhøy M, Šaltytė Benth J, Rostoft S, Selbæk G, Jensen Hjermstad M, Grønberg BH (2015) Comparing comorbidity scales: attending physician score versus the Cumulative Illness Rating Scale for Geriatrics. J Geriatr Oncol. pii: S1879-4068(15)00323-9
Extermann M, Overcash J, Lyman GH, Parr J, Balducci L (1998) Comorbidity and functional status are independent in older cancer patients. J Clin Oncol 16:1582–1587
Marvin K, Parham K (2015) Differentiated thyroid cancer in people aged 85 and older. J Am Geriatr Soc 63:932–937
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors indicate that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Weißenborn, I., Ritter, J., Geißler, K. et al. Comparison of old (75–79 years) to very old (80+ years) hospitalized otorhinolaryngology patients. Eur Arch Otorhinolaryngol 273, 2833–2842 (2016). https://doi.org/10.1007/s00405-016-4016-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-016-4016-3