Abstract
Background
Older women are poorly represented in trials evaluating chemotherapy for breast cancer (BC). This study aimed to describe survival and associated factors among elderly women receiving chemotherapy for non-metastatic BC.
Methods
This was a population-based cohort study including women ≥ 70 years old diagnosed with invasive, non-metastatic BC from 2010 to 2017 in SEER. Among those who received chemotherapy, overall survival (OS) was determined using Kaplan–Meier curves and hazard ratios were reported with 95% confidence intervals (CIs). Adjustment was made for available confounders. Co-morbidity is not available in SEER. BC-specific survival (BCSS) and subdistribution hazard ratios were determined using competing risks analysis.
Results
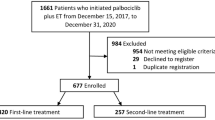
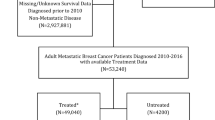
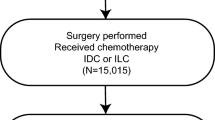
The cohort consisted of 109,239 women aged 70+, of whom 17,961 (16%) received chemotherapy. Chemotherapy patients were younger (median 73.0 years vs. 77.0), had more advanced disease (25% stage III vs. 5.2%), and were more likely to receive mastectomy (50% vs. 33%). Among chemotherapy patients, 5-year OS was 77.8% (95% CI 76.9–78.6%), and for women 80+ was 60.2% (95% CI 57.5–63.1%). More recent diagnoses, no previous history of cancer, and receipt of radiotherapy were all associated with improved BCSS. Conversely, older age, higher tumour grade, advanced stage, and human epidermal growth factors receptor (HER)2 negative tumours were associated with worse BCSS. 56% of deaths were due to BC, and women aged 80+ had worse BCSS compared to those aged 70–79 (adjusted sdHR 1.62, 95% CI 1.43–1.84).
Conclusions
Elderly women with advanced disease can achieve good survival after chemotherapy for non-metastatic BC. Those with HER2+ disease have superior survival, reinforcing benefit in this population.




Similar content being viewed by others
Data availability
Due to the nature of this research, participants of this study did not explicitly agree for their data to be shared publicly, so supporting data are not available.
Code availability
Available upon request.
References
Female breast cancer—cancer stat facts. SEER. https://seer.cancer.gov/statfacts/html/breast.html. Accessed 12 April 2019
Siegel RL, Miller KD, Jemal A (2019) Cancer statistics, 2019. CA Cancer J Clin 69:7–34. https://doi.org/10.3322/caac.21551
Lagacé F, Ghazawi FM, Le M et al (2019) Analysis of incidence, mortality trends, and geographic distribution of breast cancer patients in Canada. Breast Cancer Res Treat 178:683–691. https://doi.org/10.1007/s10549-019-05418-2
Goodwin JS, Hunt WC, Samet JM (1993) Determinants of cancer therapy in elderly patients. Cancer 72:594–601. https://doi.org/10.1002/1097-0142(19930715)72:2%3c594::aid-cncr2820720243%3e3.0.co;2-#
DeMichele A, Putt M, Zhang Y et al (2003) Older age predicts a decline in adjuvant chemotherapy recommendations for patients with breast carcinoma: evidence from a tertiary care cohort of chemotherapy-eligible patients. Cancer 97:2150–2159. https://doi.org/10.1002/cncr.11338
Mandelblatt JS, Cai L, Luta G et al (2017) Frailty and long-term mortality of older breast cancer patients: CALGB 369901 (Alliance). Breast Cancer Res Treat 164:107–117. https://doi.org/10.1007/s10549-017-4222-8
Owusu C, Lash TL, Silliman RA (2007) Effect of undertreatment on the disparity in age-related breast cancer-specific survival among older women. Breast Cancer Res Treat 102:227–236. https://doi.org/10.1007/s10549-006-9321-x
Dotan E, Walter LC, Browner IS et al (2021) NCCN guidelines® insights: older adult oncology, version 1.2021: featured updates to the NCCN guidelines. J Natl Compr Canc Netw 19:1006–1019. https://doi.org/10.6004/jnccn.2021.0043
Muss HB, Polley M-YC, Berry DA et al (2019) Randomized trial of standard adjuvant chemotherapy regimens versus Capecitabine in older women with early breast cancer: 10-year update of the CALGB 49907 trial. J Clin Oncol 37:2338–2348. https://doi.org/10.1200/JCO.19.00647
Crozier JA, Pezzi TA, Hodge C et al (2020) Addition of chemotherapy to local therapy in women aged 70 years or older with triple-negative breast cancer: a propensity-matched analysis. Lancet Oncol 21:1611–1619. https://doi.org/10.1016/S1470-2045(20)30538-6
Tamirisa N, Lin H, Shen Y et al (2020) Association of chemotherapy with survival in elderly patients with multiple comorbidities and estrogen receptor-positive, node-positive breast cancer. JAMA Oncol 23:56–89. https://doi.org/10.1001/jamaoncol.2020.2388
Janeva S, Zhang C, Kovács A et al (2020) Adjuvant chemotherapy and survival in women aged 70 years and older with triple-negative breast cancer: a Swedish population-based propensity score-matched analysis. Lancet Healthy Longev 1:e117–e124. https://doi.org/10.1016/S2666-7568(20)30018-0
Gajra A, McCall L, Muss HB et al (2018) The preference to receive chemotherapy and cancer-related outcomes in older adults with breast cancer CALGB 49907 (Alliance). J Geriatr Oncol 9:221–227. https://doi.org/10.1016/j.jgo.2018.02.003
Harder H, Ballinger R, Langridge C et al (2013) Adjuvant chemotherapy in elderly women with breast cancer: patients’ perspectives on information giving and decision making. Psychooncology 22:2729–2735. https://doi.org/10.1002/pon.3338
Simes RJ, Coates AS (2001) Patient preferences for adjuvant chemotherapy of early breast cancer: how much benefit is needed? JNCI Monogr 2001:146152
Srokowski TP, Fang S, Hortobagyi GN, Giordano SH (2009) Impact of diabetes mellitus on complications and outcomes of adjuvant chemotherapy in older patients with breast cancer. J Clin Oncol 27:2170–2176. https://doi.org/10.1200/JCO.2008.17.5935
Aaldriks AA, van der Geest LGM, Giltay EJ et al (2013) Frailty and malnutrition predictive of mortality risk in older patients with advanced colorectal cancer receiving chemotherapy. J Geriatr Oncol 4:218–226. https://doi.org/10.1016/j.jgo.2013.04.001
Pressoir M, Desné S, Berchery D et al (2010) Prevalence, risk factors and clinical implications of malnutrition in French Comprehensive Cancer Centres. Br J Cancer 102:966–971. https://doi.org/10.1038/sj.bjc.6605578
Raji MA, Kuo Y-F, Freeman JL, Goodwin JS (2008) Effect of a dementia diagnosis on survival of older patients after a diagnosis of breast, colon, or prostate cancer: implications for cancer care. Arch Intern Med 168:2033–2040. https://doi.org/10.1001/archinte.168.18.2033
Canoui-Poitrine F, Reinald N, Laurent M et al (2016) Geriatric assessment findings independently associated with clinical depression in 1092 older patients with cancer: the ELCAPA Cohort Study. Psychooncology 25:104–111. https://doi.org/10.1002/pon.3886
Wang T, Baskin AS, Dossett LA (2020) Deimplementation of the choosing wisely recommendations for low-value breast cancer surgery: a systematic review. JAMA Surg. https://doi.org/10.1001/jamasurg.2020.0322
Sun J, Mathias BJ, Sun W et al (2021) Is it wise to omit sentinel node biopsy in elderly patients with breast cancer? Ann Surg Oncol 28:320–329. https://doi.org/10.1245/s10434-020-08759-1
Chagpar AB, Horowitz N, Sanft T et al (2017) Does lymph node status influence adjuvant therapy decision-making in women 70 years of age or older with clinically node negative hormone receptor positive breast cancer? Am J Surg 214:1082–1088. https://doi.org/10.1016/j.amjsurg.2017.07.036
Biganzoli L, Wildiers H, Oakman C et al (2012) Management of elderly patients with breast cancer: updated recommendations of the International Society of Geriatric Oncology (SIOG) and European Society of Breast Cancer Specialists (EUSOMA). Lancet Oncol 13:e148-160. https://doi.org/10.1016/S1470-2045(11)70383-7
Saleh RR, Nadler MB, Desnoyers A et al (2020) Influence of competing risks on estimates of recurrence risk and breast cancer-specific mortality in analyses of the Early Breast Cancer Trialists Collaborative Group. Sci Rep 10:4091. https://doi.org/10.1038/s41598-020-61093-0
Doll KM, Rademaker A, Sosa JA (2018) Practical guide to surgical data sets: surveillance, epidemiology, and end results (SEER) database. JAMA Surg 153:588
SEER incidence database—SEER data & software. SEER. https://seer.cancer.gov/data/index.html. Accessed 26 Feb 2019
von Elm E, Altman DG, Egger M et al (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet (London, England) 370:1453–1457. https://doi.org/10.1016/S0140-6736(07)61602-X
Summary staging manual—2018. SEER. https://seer.cancer.gov/tools/ssm/index.html. Accessed 8 Feb 2022
Months survived based on complete dates. SEER. https://seer.cancer.gov/survivaltime/index.html. Accessed 29 June 2020
SEER cause of death recode 1969+ (9/17/2004)—SEER data reporting tools. SEER. https://seer.cancer.gov/codrecode/1969_d09172004/index.html. Accessed 29 June 2020
Lv M, Yuan P, Ma Y et al (2021) Evaluation of whether adjuvant chemotherapy can be safely omitted for older female patients with ER-positive, HER2-negative N1 breast cancer: a study based on the SEER database. Ann Transl Med 9:1082. https://doi.org/10.21037/atm-21-3097
Iqbal J, Ginsburg O, Rochon PA et al (2015) Differences in breast cancer stage at diagnosis and cancer-specific survival by race and ethnicity in the United States. JAMA 313:165–173. https://doi.org/10.1001/jama.2014.17322
Silber JH, Rosenbaum PR, Clark AS et al (2013) Characteristics associated with differences in survival among black and white women with breast cancer. JAMA 310:389–397. https://doi.org/10.1001/jama.2013.8272
Osei-Twum J-A, Gedleh S, Lofters A, Nnorom O (2021) Differences in breast cancer presentation at time of diagnosis for black and white women in high resource settings. J Immigr Minor Health 23:1305–1342. https://doi.org/10.1007/s10903-021-01161-3
DeSantis C, Jemal A, Ward E (2010) Disparities in breast cancer prognostic factors by race, insurance status, and education. Cancer Causes & Control: CCC 21:1445–1450. https://doi.org/10.1007/s10552-010-9572-z
Williams DR, Mohammed SA, Shields AE (2016) Understanding and effectively addressing breast cancer in African American women: unpacking the social context. Cancer 122:2138–2149. https://doi.org/10.1002/cncr.29935
Flanagin A, Frey T, Christiansen SL (2021) Updated guidance on the reporting of race and ethnicity in medical and science journals. JAMA 326:621–627. https://doi.org/10.1001/jama.2021.13304
Vyas DA, Eisenstein LG, Jones DS (2020) Hidden in plain sight—reconsidering the use of race correction in clinical algorithms. N Engl J Med 383:874–882. https://doi.org/10.1056/NEJMms2004740
Hu C-Y, Xing Y, JaniceN C, Chang GJ (2013) Assessing the utility of cancer-registry-processed cause of death in calculating cancer-specific survival. Cancer 119:1900–1907. https://doi.org/10.1002/cncr.27968
Austin PC, Lee DS, Fine JP (2016) Introduction to the analysis of survival data in the presence of competing risks. Circulation 133:601–609. https://doi.org/10.1161/CIRCULATIONAHA.115.017719
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Castelo, M., Lu, J., Paszat, L. et al. Long-term survival in elderly women receiving chemotherapy for non-metastatic breast cancer: a population-based analysis. Breast Cancer Res Treat 194, 629–641 (2022). https://doi.org/10.1007/s10549-022-06646-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-022-06646-9