Abstract
Purpose
To evaluate the long-term local control, failure patterns, and toxicities after individualized clinical target volume (CTV) delineation in unilateral nasopharyngeal carcinoma (NPC) treated with intensity-modulated radiotherapy (IMRT).
Methods
Unilateral NPC was defined as a nasopharyngeal mass confined to one side of the nasopharynx and did not exceed the midline. From November 2003 to December 2017, 95 patients were retrospectively included. All patients received IMRT. The CTVs were determined based on the distance from the gross tumor. The contralateral para-pharyngeal space and skull base orifices were spared from irradiation.
Results
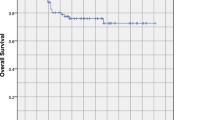
There were three local recurrences and eight regional recurrences in 10 patients during an 84-month follow-up. All local recurrences were within PGTVnx, and all in-field recurrences. No recurrences were found in traditional high-risk areas including contralateral the para-pharyngeal space and skull base orifices. The 10-year local-recurrence-free survival, regional-recurrence-free survival and overall survival were 96.2%, 90.5% and 84.7%, respectively. The dosimetry parameters of the tumor-contralateral organs were all lower than the values of the tumor-ipsilateral side (P < 0.05). The late toxicities occurred mainly in the tumor-ipsilateral organs, including radiation-induced temporal lobe injury, impaired visuality, hearing loss and subcutaneous fibrosis.
Conclusion
Individualized CTV delineation in unilateral NPC could yield excellent long-term local control with limited out-of-field recurrences, reduced dose to tumor- contralateral organs and mild late toxicities, which is worthy of further exploration.




Similar content being viewed by others
Availability of data and material
The datasets used and/or analyzed during the current study were uploaded onto the Research Data Deposit public platform (www.researchdata.org.cn), with the RDD approval number RDDB2020001032.
Abbreviations
- IMRT:
-
Intensity-modulated radiotherapy
- NPC:
-
Nasopharyngeal carcinoma
- LCR:
-
Local control rate
- GTV:
-
Gross tumor volume
- CTV:
-
Clinical target volume
- TLI:
-
Temporal lobe injury
- SYSUCC:
-
Sun Yat-sen University Cancer Center
- ENS:
-
Electronic nasopharyngoscope
- MRI:
-
Magnetic resonance imaging
- PS:
-
Performance status
- AJCC:
-
American Joint Committee on Cancer
- CCRT:
-
Concurrent chemo-radiotherapy
- IC:
-
Induction chemotherapy
- CT:
-
Computed tomography
- OARs:
-
Organs at risk
- ICRU:
-
The International Commission on Radiation Units and Measurement
- CTV1:
-
High-risk clinical target volume
- CTV2:
-
Low-risk clinical target volume
- RTOG:
-
Radiation Therapy Oncology Group
- PTV:
-
Planning target volume
- ECT:
-
Emission computed tomography
- PET/CT:
-
Positron emission tomography-computed tomography
- LRFS:
-
Local-recurrence-free survival
- OS:
-
Overall survival
- RRFS:
-
Regional relapse-free survival
- DMFS:
-
Distant metastasis-free survival
- PFS:
-
Progression-free survival
- Dmean:
-
Mean dose
- Dmin:
-
Minimum dose
- Dmax:
-
Maximum dose
References
Au KH, Ngan Roger KC, Ng Alice WY et al (2018) Treatment outcomes of nasopharyngeal carcinoma in modern era after intensity modulated radiotherapy (IMRT) in Hong Kong: A report of 3328 patients (HKNPCSG 1301 study). Oral Oncol 77:16–21
Chen Q-Y, Wen Y-F, Guo L et al (2011) Concurrent chemoradiotherapy vs radiotherapy alone in stage II nasopharyngeal carcinoma: phase III randomized trial. J Natl Cancer Inst 103:1761–1770
Chen L, Zhang Y, Lai S-Z et al (2019) 10-year results of therapeutic ratio by intensity-modulated radiotherapy versus two-dimensional radiotherapy in patients with nasopharyngeal carcinoma. Oncologist 24:e38–e45
Clifford CKS, Ozyigit G, Tran BN et al (2003) Patterns of failure in patients receiving definitive and postoperative IMRT for head-and-neck cancer. Int J Radiat Oncol Biol Phys 55:312–321
Dawson LA, Anzai Y, Marsh L et al (2000) Patterns of local-regional recurrence following parotid-sparing conformal and segmental intensity-modulated radiotherapy for head and neck cancer. Int J Radiat Oncol Biol Phys 46:1117–1126
Grégoire V, Evans M, Le Q-T et al (2018) Delineation of the primary tumour Clinical Target Volumes (CTV-P) in laryngeal, hypopharyngeal, oropharyngeal and oral cavity squamous cell carcinoma: AIRO, CACA, DAHANCA, EORTC, GEORCC, GORTEC, HKNPCSG, HNCIG, IAG-KHT, LPRHHT, NCIC CTG, NCRI, NRG Oncology, PHNS, SBRT, SOMERA, SRO, SSHNO TROG Consensus Guidelines. Radiother Oncol 126:3–24
Lai S-Z, Li W-F, Chen L et al (2011) How does intensity-modulated radiotherapy versus conventional two-dimensional radiotherapy influence the treatment results in nasopharyngeal carcinoma patients? Int J Radiat Oncol Biol Phys 80:661–668
Lee N, Xia P, Quivey Jeanne M et al (2002) Intensity-modulated radiotherapy in the treatment of nasopharyngeal carcinoma: an update of the UCSF experience. Int J Radiat Oncol Biol Phys 53:12–22
Lee Anne W, Ng WT, Pan JJ et al (2018) International guideline for the delineation of the clinical target volumes (CTV) for nasopharyngeal carcinoma. Radiother Oncol 126:25–36
Li X-Y, Chen Q-Y, Sun X-S et al (2019) Ten-year outcomes of survival and toxicity for a phase III randomised trial of concurrent chemoradiotherapy versus radiotherapy alone in stage II nasopharyngeal carcinoma. Eur J Cancer 110:24–31
Liu Y-P, Wen Y-H, Tang J et al (2021) Endoscopic surgery compared with intensity-modulated radiotherapy in resectable locally recurrent nasopharyngeal carcinoma: a multicentre, open-label, randomised, controlled, phase 3 trial. Lancet Oncol 22:381–390
McDowell Lachlan J, Rock K, Xu W et al (2018) Long-Term late toxicity, quality of life, and emotional distress in patients with nasopharyngeal carcinoma treated with intensity modulated radiation therapy. Int J Radiat Oncol Biol Phys 102:340–352
Miao J, Di M, Chen B et al (2020) A prospective 10-year observational study of reduction of radiation therapy clinical target volume and dose in early-stage nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys 107:672–682
National Comprehensive Cancer Network (2018) (NCCN) Clinical Practice Guidelines in Oncology. Head and Neck Cancer, Version 1. 2018. https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf. Accessed 15 Feb 2018
Ng WT, Soong YL, Ahn YC et al (2021) International recommendations on reirradiation by intensity modulated radiation therapy for locally recurrent nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys 110:682–695
Sanford Nina N, Jackson L, Lam Miranda B et al (2019) Individualization of clinical target volume delineation based on stepwise spread of nasopharyngeal carcinoma: outcome of more than a decade of clinical experience. Int J Radiat Oncol Biol Phys 103:654–668
Su S-F, Han F, Zhao C et al (2012) Long-term outcomes of early-stage nasopharyngeal carcinoma patients treated with intensity-modulated radiotherapy alone. Int J Radiat Oncol Biol Phys 82:327–333
Sun Y, Yu X-L, Luo W et al (2014) Recommendation for a contouring method and atlas of organs at risk in nasopharyngeal carcinoma patients receiving intensity-modulated radiotherapy. Radiother Oncol 110:390–397
Sun Y, Yu X-L, Zhang G et al (2016) Reduction of clinical target volume in patients with lateralized cancer of the nasopharynx and without contralateral lymph node metastasis receiving intensity-modulated radiotherapy. Head Neck 38(S1):E468–E472
Wang L, Wu Z, Xie D et al (2019) Reduction of target volume and the corresponding dose for the tumor regression field after induction chemotherapy in locoregionally advanced nasopharyngeal carcinoma. Cancer Res Treat 51:685–695
Wu L-R, Liu Y-T, Jiang N et al (2017) Ten-year survival outcomes for patients with nasopharyngeal carcinoma receiving intensity-modulated radiotherapy: an analysis of 614 patients from a single center. Oral Oncol 69:26–32
Wu Z, Wang L, Xie D-H et al (2021) Failure patterns and prognostic factors for cervical node-negative nasopharyngeal carcinoma in the intensity-modulated radiotherapy era. Asia Pac J Clin Oncol 17:330–337
Xie D, Cheng W, Lv S et al (2019) Target delineation and dose prescription of adaptive replanning intensity-modulated radiotherapy for nasopharyngeal carcinoma. Cancer Commun (lond) 39:18
Zeng L, Huang S-M, Tian Y-M et al (2015) Normal tissue complication probability model for radiation-induced temporal lobe injury after intensity-modulated radiation therapy for nasopharyngeal carcinoma. Radiology 276:243–249
Zhang F, Zhang Y, Li W-F et al (2015) Efficacy of concurren chemotherapy for intermediate risk NPC in the intensity-modulated radiotherapy era: a propensity-matched analysis. Sci Rep 5:17378
Acknowledgements
We thank International Science Editing (http://www.internationalscienceediting.com) for editing this manuscript.
Funding
The authors declare that they had no funding for this study.
Author information
Authors and Affiliations
Contributions
DHX, ZW, WZL, YS, and YQH designed the study. DHX, ZW, YS, TXL, JM, CZ, NJC, WQC, LW, and SWL delineated the targets and performed radiation treatment DHX, ZW, WZL, WQC, YLT, LW, SWL, FFL, and SMH acquired data DHX, ZW, WZL, analyzed and interpreted the data. DHX, ZW, WZL, and YS wrote the manuscript, and revised the manuscript. All authors have reviewed the manuscript and approved the final version.
Corresponding authors
Ethics declarations
Conflicts of interest/Competing interests
The authors declare that they have no competing interests.
Ethics approval
Retrospective ethical approval was obtained from the institutional ethics committee of the Sun Yat‑sen University Cancer Center, with the approval number B2019-169–01. Written informed treatment consents were required from all patients with respect to chemotherapy and/or radiotherapy.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xie, DH., Wu, Z., Li, WZ. et al. Individualized clinical target volume delineation and efficacy analysis in unilateral nasopharyngeal carcinoma treated with intensity-modulated radiotherapy (IMRT): 10-year summary. J Cancer Res Clin Oncol 148, 1931–1942 (2022). https://doi.org/10.1007/s00432-022-03974-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-03974-7