Abstract
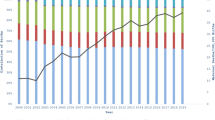
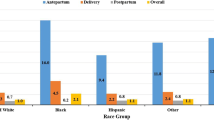
Persistent racial/ethnic disparities in maternal morbidity and mortality in the United States have been documented and are complex and multifaceted. Furthering the understanding of the origins of these differences is a public health priority. This chapter explores racial/ethnic differences in maternal morbidity (maternal transfusion, ruptured uterus, unplanned hysterectomy, and ICU admission) using new data from birth certificates for 41 states and the District of Columbia that adopted the 2003 U.S. Standard Certificate of Live Birth . Racial/ethnic differences in maternal mortality are examined using new data from death certificates on the three periods of maternal death relative to the pregnancy–pregnant at the time of death, died with 42 days of an ended pregnancy, or died 43 days to 1 year after an ended pregnancy for the 39 states and the District of Columbia that have adopted the 2003 U.S. Standard Certificate of Death. Rates (per 100,000 live births) of maternal morbidity and mortality were estimated for non-Hispanic white, non-Hispanic black, non-Hispanic Asian , and Hispanic women. Racial/ethnic disparities in maternal morbidity were examined in logistic regression models after adjusting for demographic, health/clinical, and healthcare access confounders. Racial/ethnic differences were evident for all four morbidities and in all three periods of maternal mortality but were larger for maternal mortality than morbidity. Non-Hispanic black women had among the highest rates for both morbidity and mortality whereas Hispanic women had among the lowest rates for mortality. These new data will be an important resource in tracking trends and differentials in maternal morbidity and mortality.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
American College of Obstetricians and Gynecologists. (2006). ACOG practice bulletin no. 76: Postpartum hemorrhage. Obstetrics and Gynecology, 108, 1039–1047.
Arias, E. (2010). United States life tables by Hispanic origin. Vital and Health Statistics, 2(152), 1–33.
Arias, E., Schauman, W. S., Eschbach, K., Sorlie, P. D., & Backlund, E. (2008). The validity of race and Hispanic origin reporting on death certificates in the United States. Vital and health statistics, 2(148), 1–23.
Bateman, B. T., Mhyre, J. M., Callaghan, W. M., & Kuklina, E. V. (2012). Peripartum hysterectomy in the United States: nationwide 14 year experience. American Journal of Obstetrics and Gynecology, 206(1), 63.e1–63.e8. doi:10.1016/j.ajog.2011.07.030
Berg, C. J., Callaghan, W. M., Syverson, C., & Henderson, Z. (2010). Pregnancy-related mortality in the United States, 1998 to 2005. Obstetrics and Gynecology, 116(6), 1302–1309. doi:10.1097/AOG.0b013e3181fdfb11
Bryant, A. S., Worjoloh, A., Caughey, A. B., & Washington, A. E. (2010). Racial/ethnic disparities in obstetric outcomes and care: prevalence and determinants. American Journal of Obstetrics and Gynecology, 202(4), 335–343. doi:10.1016/j.ajog.2009.10.864
Buescher, P. A., Taylor, K. P., Davis, M. H., & Bowling, J. M. (1993). The quality of the new birth certificate data: a validation study in North Carolina. American Journal of Public Health, 83(8), 1163–1165.
Callaghan, W. M., Grobman, W. A., Kilpatrick, S. J., Main, E. K., & D’Alton, M. (2014). Facility-based identification of women with severe maternal morbidity: it is time to start. Obstetrics and Gynecology, 123(5), 978–981. doi:10.1097/AOG.0000000000000218
Campbell, K. H., Savitz, D., Werner, E. F., Pettker, C. M., Goffman, D., Chazotte, C., et al. (2013). Maternal morbidity and risk of death at delivery hospitalization. Obstetrics and Gynecology, 122(3), 627–633. doi:10.1097/AOG
Carr, A., Kershaw, T., Brown, H., Allen, T., & Small, M. (2013). Hypertensive disease in pregnancy: An examination of ethnic differences and the Hispanic paradox. Journal of Neonatal-Perinatal Medicine, 6(1), 11–15. doi:10.3233/NPM-1356111
Center for Medicare and Medicaid Services. (2015). Pregnant women. Available from: http://www.medicaid.gov/medicaid-chip-program-information/by-population/pregnant-women/pregnant-women.html
Centers for Disease Control and Prevention. (2015a). Pregnancy mortality surveillance system. Available at: http://www.cdc.gov/reproductivehealth/MaternalInfantHealth/PMSS.html
Centers for Disease Control and Prevention. (2015b). Severe maternal morbidity in the United States. Available at: http://www.cdc.gov/reproductivehealth/MaternalInfantHealth/SevereMaternalMorbidity.html
Creanga, A. A., Bateman, B. T., Kuklina, E. V., & Callaghan, W. M. (2014b). Racial and ethnic disparities in severe maternal morbidity: A multistate analysis, 2008–2010. American Journal of Obstetrics and Gynecology, 210(5), 435.e1–435.e8. doi:10.1016/j.ajog.2013.11.039
Creanga, A. A., Berg, C. J., Ko, J. Y., Farr, S. L., Tong, V. T., Bruce, F. C., et al. (2014a). Maternal mortality and morbidity in the United States: Where are we now? Journal of Women’s Health, 23(1), 3–9. doi:10.1089/jwh.2013.4617
Creanga, A. A., Berg, C. J., Syverson, C., Seed, K., Bruce, F. C., & Callaghan, W. M. (2012). Race, ethnicity, and nativity differentials in pregnancy-related mortality in the United States: 1993–2006. Obstetrics and Gynecology, 120(2 Pt 1), 261–268. doi:10.1097/AOG.0b013e31825cb87a
Curtin, S. C., Gregory, K. D., Korst, L. M., & Uddin, S. F. (2015). Maternal morbidity for vaginal and cesarean deliveries, according to previous Cesarean History: New data from the birth certificate, 2013. National Vital Statistics Reports, 64(4), 1–13, back cover.
Firoz, T., Chou, D., von Dadelszen, P., Agrawal, P., Vanderkruik, R., & Tuncalp, O. (2013). Measuring maternal health: focus on maternal morbidity. Bulletin of the World Health Organization, 91(10), 794–796. doi:10.2471/BLT.13.117564
Fridman, M., Korst, L. M., Chow, J., Lawton, E., Mitchell, C., & Gregory, K. D. (2014). Trends in maternal morbidity before and during pregnancy in California. American Journal of Public Health, 104(Suppl 1), S49–S57. doi:10.2105/AJPH.2013.301583
Geller, S. E., Rosenberg, D., Cox, S. M., Brown, M. L., Simonson, L., Driscoll, C. A., et al. (2004). The continuum of maternal morbidity and mortality: Factors associated with severity. American Journal of Obstetrics and Gynecology, 191(3), 939–944. doi:10.1016/j.ajog.2004.05.099
Gray, K. E., Wallace, E. R., Nelson, K. R., Reed, S. D., & Schiff, M. A. (2012). Population-based study of risk factors for severe maternal morbidity. Paediatric and Perinatal Epidemiology, 26(6), 506–514. doi:10.1111/ppe.12011
Grobman, W. A., Bailit, J. L., Rice, M. M., Wapner, R. J., Reddy, U. M., Varner, M. W., et al. (2015). Racial and ethnic disparities in maternal morbidity and obstetric care. Obstetrics and Gynecology, 125(6), 1460–1467. doi:10.1097/AOG.0000000000000735
Guise, J. M., Berlin, M., McDonagh, M., Osterweil, P., Chan, B., & Helfand, M. (2004). Safety of vaginal birth after cesarean: A systematic review. Obstetrics and Gynecology, 103(3), 420–429. doi:10.1097/01.AOG.0000116259.41678.f1
Horon, I. L., & Cheng, D. (2011). Effectiveness of pregnancy check boxes on death certificates in identifying pregnancy-associated mortality. Public Health Reports, 126(2), 195–200.
Hoyert, D. L. (2007). Maternal mortality and related concepts. Vital and Health Statistics, 3(33), 1–13.
MacKay, A. P., Berg, C. J., Duran, C., Chang, J., & Rosenberg, H. (2005). An assessment of pregnancy-related mortality in the United States. Paediatric and Perinatal Epidemiology, 19(3), 206–214. doi:10.1111/j.1365-3016.2005.00653.x
MacKay, A. P., Berg, C. J., Liu, X., Duran, C., & Hoyert, D. L. (2011). Changes in pregnancy mortality ascertainment: United States, 1999–2005. Obstetrics and Gynecology, 118(1), 104–110. doi:10.1097/AOG.0b013e31821fd49d
MacKay, A. P., Rochat, R., Smith, J. C., & Berg, C. J. (2000). The check box: determining pregnancy status to improve maternal mortality surveillance. American Journal of Preventive Medicine, 19(1 Suppl), 35–39.
Markides, K. S., & Coreil, J. (1986). The health of Hispanics in the southwestern United States: An epidemiologic paradox. Public Health Reports, 101(3), 253–265.
Martin, J. A., Wilson, E. C., Osterman, M. J., Saadi, E. W., Sutton, S. R., & Hamilton, B. E. (2013). Assessing the quality of medical and health data from the 2003 birth certificate revision: Results from two states. National Vital Statistics Reports, 62(2), 1–19.
Murphy, S. L., Xu, J., & Kochanek, K. D. (2013). Deaths: Final data for 2010. National Vital Statistics Reports, 61(4), 1–117.
National Center for Health Statistics. (2000). Report of the panel to evaluate the U.S. Standard Certificates and Reports. Hyattsville, MD: USGPO.
National Center for Health Statistics. (2006). Guide to completing the facility worksheets for the certificate of live birth and report of fetal death (2003 revision). Hyattsville, MD: USGPO.
National Center for Health Statistics. (2009). User guide to the 2007 natality public use file. Hyattsville, MD: USGPO.
National Center for Health Statistics. (2012). User guide to the 2010 natality public use file. Hyattsville, MD: USGPO.
National Center for Health Statistics. (2013). Vital statistics, instructions for classifying multiple causes of death. NCHS instruction manual; part 2b. Hyattsville, Maryland: USGPO.
National Center for Health Statistics. (2014). User guide to the 2013 natality public use file. Hyattsville, MD: USGPO.
Office of Management and Budget. (1997). Revisions to the standards for the classification of federal data on Race and ethnicity. Fed Regist 62FR58781–58790.
Piper, J. M., Mitchel, E. F, Jr., Snowden, M., Hall, C., Adams, M., & Taylor, P. (1993). Validation of 1989 Tennessee birth certificates using maternal and newborn hospital records. American Journal of Epidemiology, 137(7), 758–768.
Rouse, D. J., MacPherson, C., Landon, M., Varner, M. W., Leveno, K. J., Moawad, A. H., et al. (2006). Blood transfusion and cesarean delivery. Obstetrics and Gynecology, 108(4), 891–897. doi:10.1097/01.AOG.0000236547.35234.8c
Senanayake, H., Dias, T., & Jayawardena, A. (2013). Maternal mortality and morbidity: Epidemiology of intensive care admissions in pregnancy. Best Practice and Research Clinical Obstetrics and Gynaecology, 27(6), 811–820. doi:10.1016/j.bpobgyn.2013.07.002
U.S. Census Bureau (2012). The Asian population: 2010. 2010 Census Briefs. C2010BR-11. Available at: http://www.census.gov/prod/cen2010/briefs/c2010br-11.pdf
Vanderkruik, R. C., Tuncalp, O., Chou, D., & Say, L. (2013). Framing maternal morbidity: WHO scoping exercise. BMC Pregnancy Childbirth, 13, 213. doi:10.1186/1471-2393-13-213
Wanderer, J. P., Leffert, L. R., Mhyre, J. M., Kuklina, E. V., Callaghan, W. M., & Bateman, B. T. (2013). Epidemiology of obstetric-related ICU admissions in Maryland: 1999–2008*. Critical Care Medicine, 41(8), 1844–1852. doi:10.1097/CCM.0b013e31828a3e24
Yap, O. W., Kim, E. S., & Laros, R. K., Jr. (2001). Maternal and neonatal outcomes after uterine rupture in labor. American Journal of Obstetrics and Gynecology, 184(7), 1576–1581.
Acknowledgments
The following persons provided helpful comments in the preparation of this manuscript: Elizabeth R. Arias, Ph. D., Amy M. Branum, Ph.D., William H. Callaghan, M.D., M.P.H., Jennifer H. Madans, Ph.D., Joyce A. Martin, M.P.H., and Hanyu Ni, M.P.H., Ph.D.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Curtin, S.C., Hoyert, D.L. (2017). Maternal Morbidity and Mortality: Exploring Racial/Ethnic Differences Using New Data from Birth and Death Certificates. In: Hoque, M., Pecotte, B., McGehee, M. (eds) Applied Demography and Public Health in the 21st Century. Applied Demography Series, vol 8. Springer, Cham. https://doi.org/10.1007/978-3-319-43688-3_7
Download citation
DOI: https://doi.org/10.1007/978-3-319-43688-3_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-43686-9
Online ISBN: 978-3-319-43688-3
eBook Packages: Social SciencesSocial Sciences (R0)